How industry should improve beyond-the-pill-programmes

Patient support programmes that extend beyond the prescription are increasingly important, with neurologists among the most experienced in such services. This article examines their views on the elements to include.
More and more pharma companies define success in terms of patient outcomes. For these companies, product delivery does not end with patients filling prescriptions. Supporting patients in adhering to their treatment plan has become increasingly important.
In neurology, in particular, such beyond-the-pill initiatives have been widespread for some time. Typically these programmes centre on specially-trained nurses calling patients and informing them about their treatment and the specifics of their medication. But digital technology is increasingly changing the game too. Patients of almost all conditions and age groups carry smartphones 24/7. This raises the question of whether traditional patient support programmes – and their reliance on phone calls – are adequate today.
A recent study1 asked 100 neurologists what a patient support programme should look like. The key finding was that support programmes should provide daily touch points with patients, rather than relying on quarterly calls. And, while physicians appreciated the pharmaceutical industry's support, they saw substantial room for improvement: instead of industry-branded programmes they would prefer them to promote independent, though industry-sponsored, programmes.
Adherence is key success factor for positive outcomes
Regarding the importance of medical adherence, there was consensus among the physicians: 100% believed that sticking to the prescribed medication plan was one of the key factors for success.
Patient support programmes should remind, educate and document
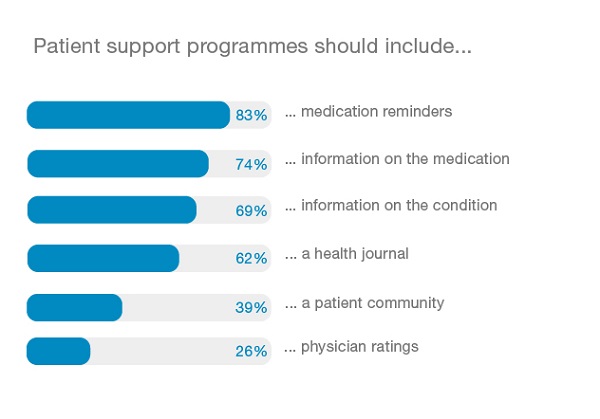
With regard to what the doctors want included in patient support programmes, 83% of those surveyed saw medication reminders as important. But to really support patients during their therapy most of the physicians required daily reminders – and thus daily interaction. Educational content was important, too: information on the medication and the condition came in second (74%) and third (69%) place, respectively. While a health journal was still important to the majority of doctors (62%), other elements, such as patient communities, were perceived as less important.
Physicians prefer independent support programmes
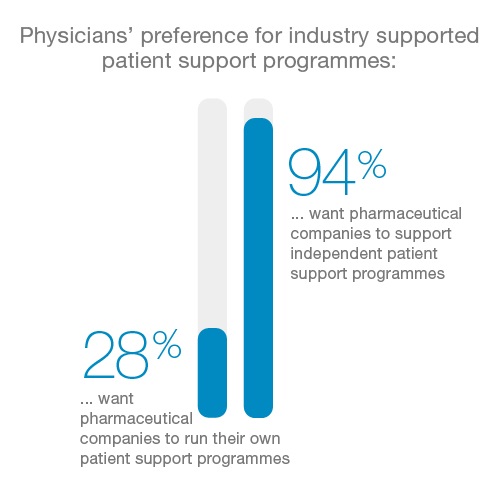
Besides patient support programmes run by the pharma industry there are also independent, non-branded programmes aiming to improve medication adherence. Asked for their preference, only 28% of physicians wanted the industry to run its own programmes. From their point of view the industry could have significantly more impact through partnering: 94% were in favour of the industry supporting medications adherence by sponsoring independent programmes.
The study's author Sebastian Gaede explained his motivation for the study to pharmaphorum: "A lot of people argue that physicians are resistant to change and not interested in digital innovation. However, our everyday experience is very different. Therefore we decided to put this widespread prejudice to the test by asking physicians directly. From my point of view, the results speak for themselves: the surveyed physicians have a very clear understanding of what it takes to support outcomes and they are open to digital technology for delivering this support."
And how does he interpret the results?
"10 years ago few physicians would have dared to ask for support programmes to have several touch points a day. Today, smartphones are the new default, shaping physicians' and patients' expectations. Reminding patients when to take every single medication is simply not possible via phone. Today's programmes neither support outcomes to the extent possible, nor do they reflect physicians' rapidly-evolving expectations towards pharma marketing."
So, based on the results, what is his recommendation to the industry?
"In an outcome-driven world, pharma should favour impact over brand visibility. Impact, on the one hand, requires the best possible offering. Therefore the industry should rethink patient support from scratch, putting smartphone-empowered patients and physicians at the centre of their considerations. On the other hand, impact requires acceptance. Therefore the industry should carefully weigh the higher acceptance of non-branded programmes versus the presumed benefits of their own, branded offerings."
1 The research was conducted by Munich-based smartpatient and can be accessed here.
About the interviewee:
Sebastian Gaede is co-founder and managing director of smartpatient, developers of the health app MyTherapy (for iOS and Android). He tweets at: @SebastianGaede
Read more on doctors' views:











