What HCPs think about health equity in cancer care

After more than a year of COVID-19 dominating health conversations, HCPs have been engaging in dialogue about continually evident disparities that many are facing in healthcare. CREATION.co's Mary Kangley explores what HCPs think about health equity in cancer care.
The topic rose to significance in the American Society of Clinical Oncology (ASCO) whereby they updated their mission statement in 2020 to “Conquering cancer through research, education, and promotion of the highest quality, equitable patient care.” Further, ASCO President Lori J. Pierce, MD, FASTRO, FASCO selected the theme for the 2021 Annual Meeting: ‘Equity: Every Patient. Every Day. Everywhere.’
While a theme constantly raised by HCPs advocating for their patients, the focus heightened in HCP online conversations at this ASCO’s 2021 virtual congress.
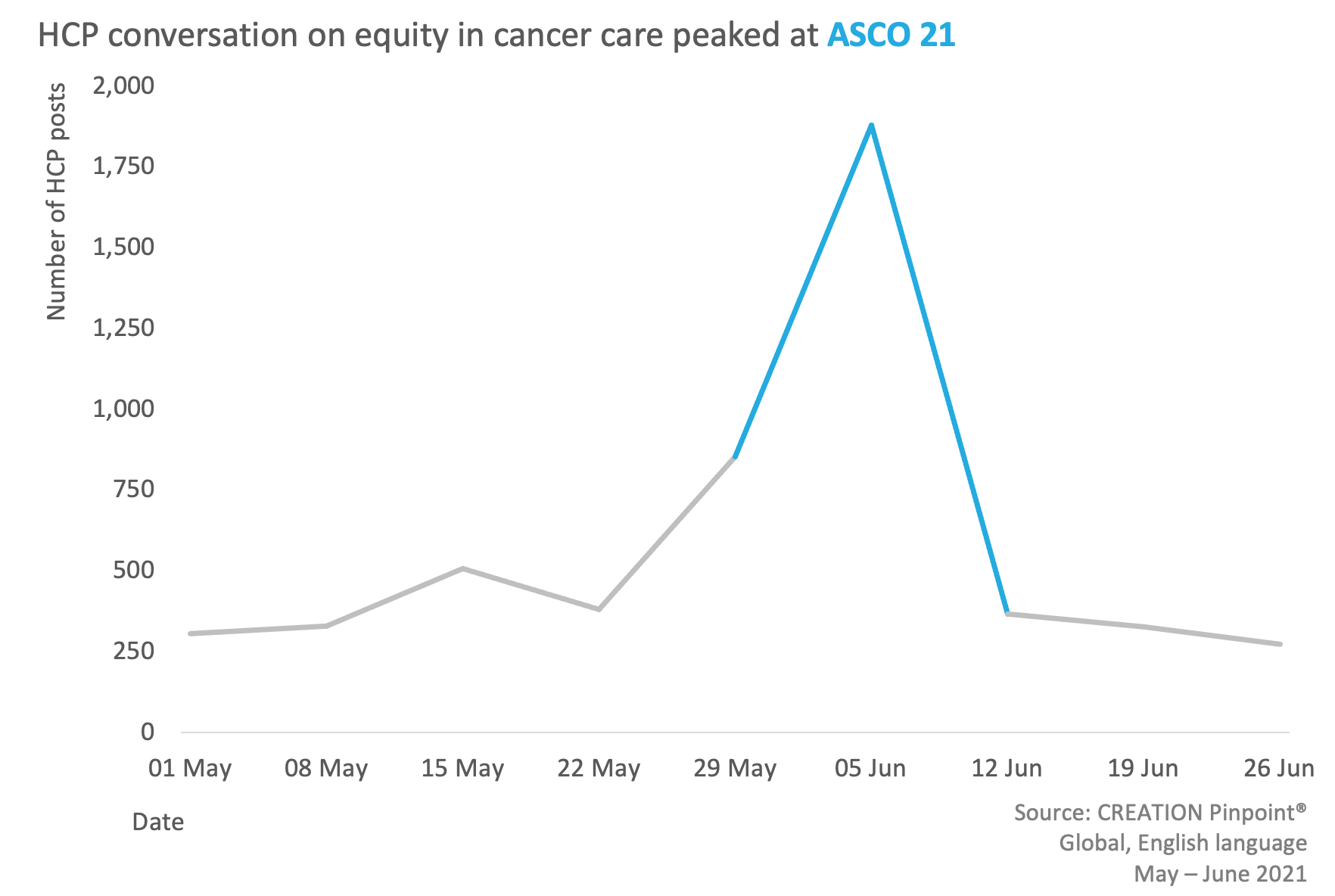
In her presidential address to open the virtual event, Lori J. Pierce, MD said “Eliminating racial and socioeconomic disparities in cancer outcomes has been a personal long-term commitment [...] but clearly today it is even more relevant than ever—since the pandemic has disproportionately affected people of color and institutional racism is finally being recognized as a societal plague that is devastating to all of us.”
Captured among HCP conversations was data from studies whose aim was to define the extent of disparities experienced across various groups as well as the input of organisations, including pharmaceutical companies, to advocate for, raise awareness and financially support these causes.
While ASCO’s president primarily addressed the issue of racism and ethic inequalities in cancer care, the discourse from the wider event reflected a variety of inequities. Financial barriers and disparities emerged as the most discussed issue.
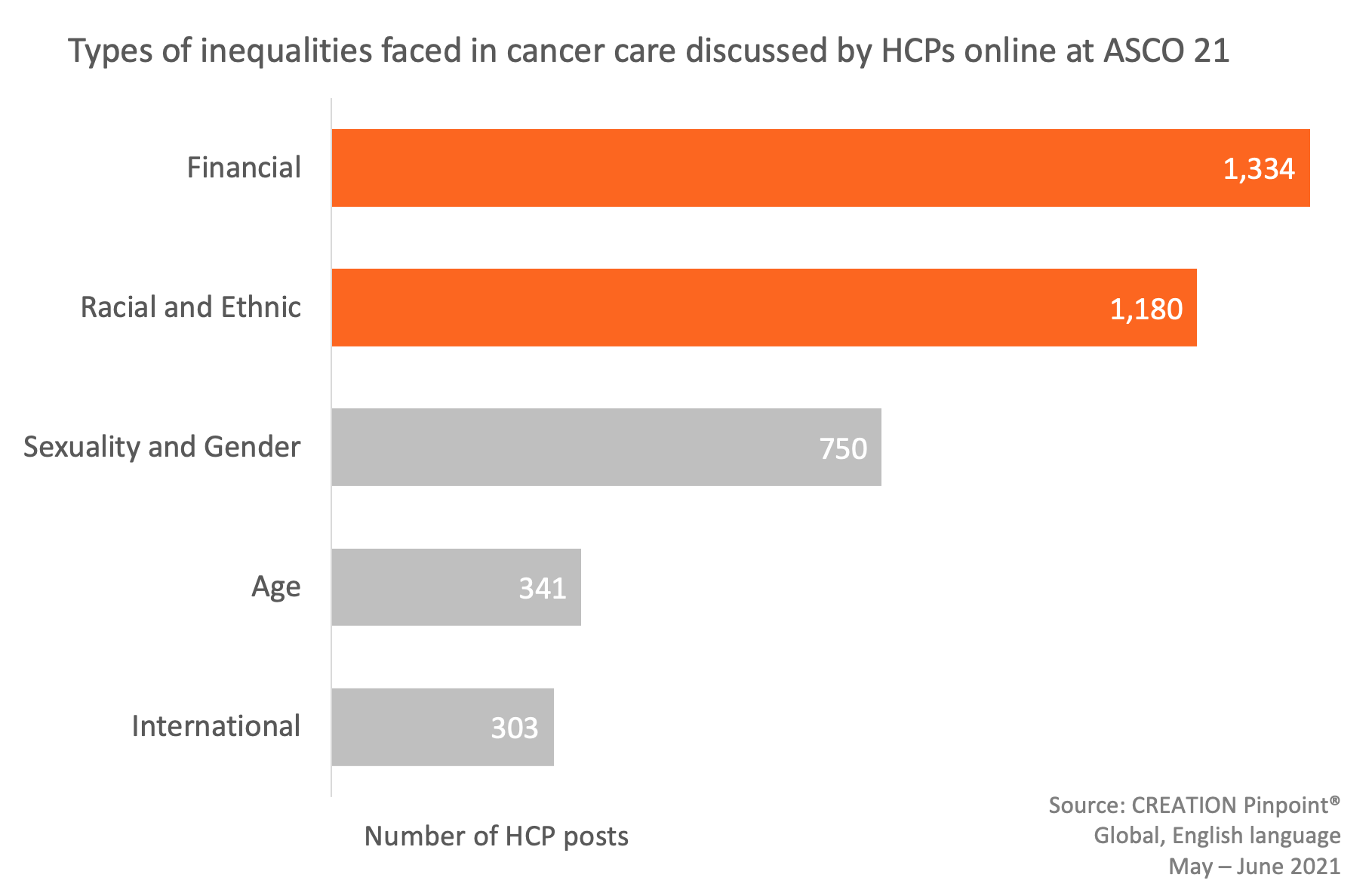
Areas of disparity
Affordability
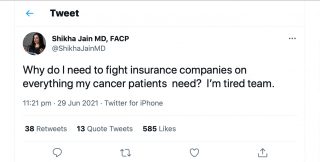
Financial disparities were the most frequently discussed hurdle for patients seeking cancer care, in over 1,000 HCP posts. Over 40% of those posts cited insurance companies alongside these access issues.
 https://twitter.com/ShikhaJainMD/status/1410000498564943872
https://twitter.com/ShikhaJainMD/status/1410000498564943872
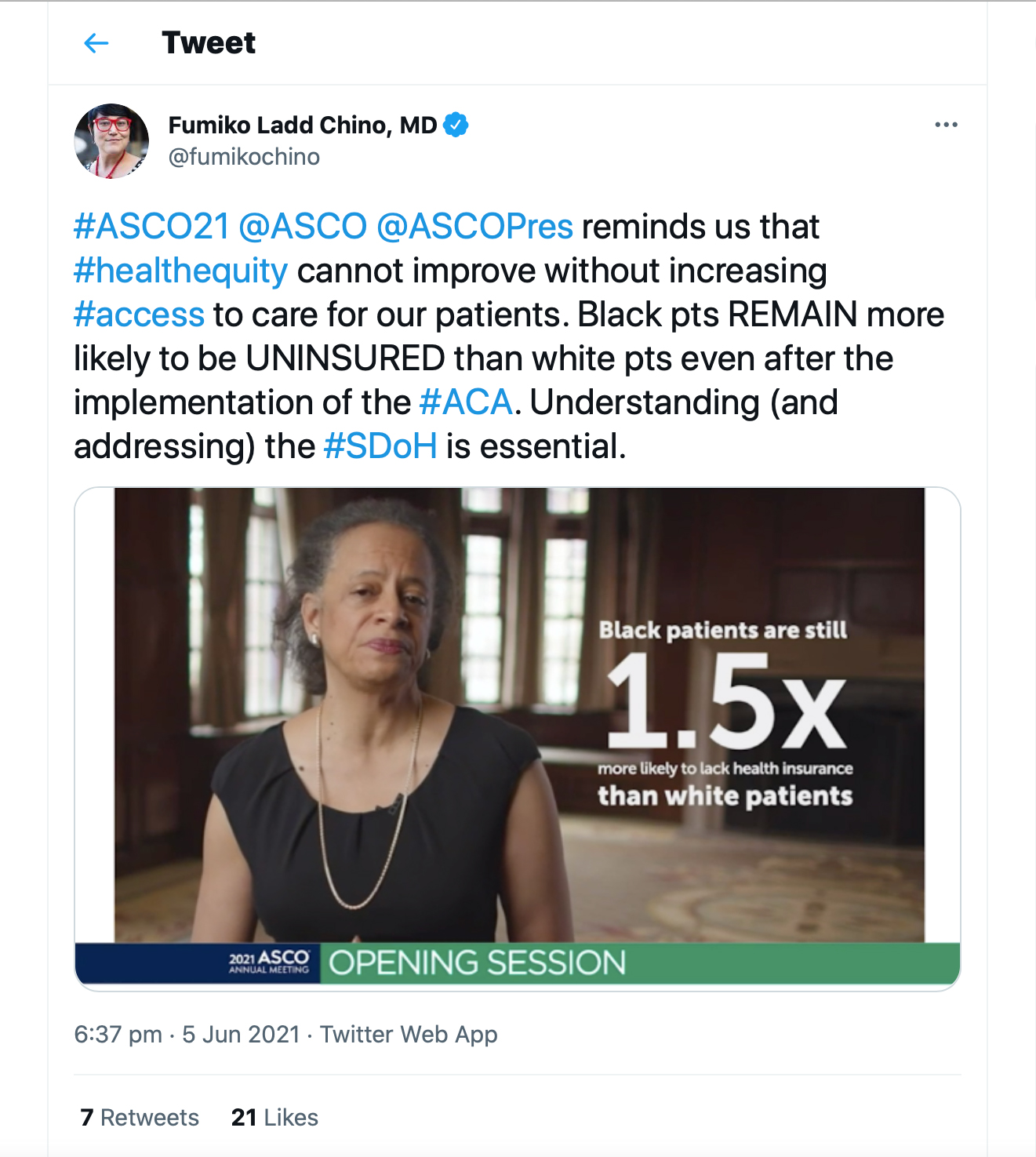
Returning to the presidential address, HCPs concentrated on racial asymmetry in insurance coverage in the US, even despite the implementation of the Affordable Care Act (ACA). Alongside others, radiation oncologist Fumiko Ladd Chino, demanded more understanding and the addressing of social determinants of health (SDoH).
 https://twitter.com/fumikochino/status/1401231731672428546
https://twitter.com/fumikochino/status/1401231731672428546
Beyond monetary concerns, each of the inequalities listed above affects various aspects of a patient's journey. From before diagnosis with check-ups and screening to trial enrollment to assess drug efficacy, we will explore how HCPs discuss this aspect of cancer care.
Screening and Diagnosis
It is known that inequalities exist across entire health systems, affecting patients throughout their journeys from screening and diagnosis to treatment expenses. HCPs shared their experiences and opinions on these obstacles, in various cancer types. Lung cancer arose as the most discussed diagnosis, a prominence which proportionally increased when in relation to screening and testing.
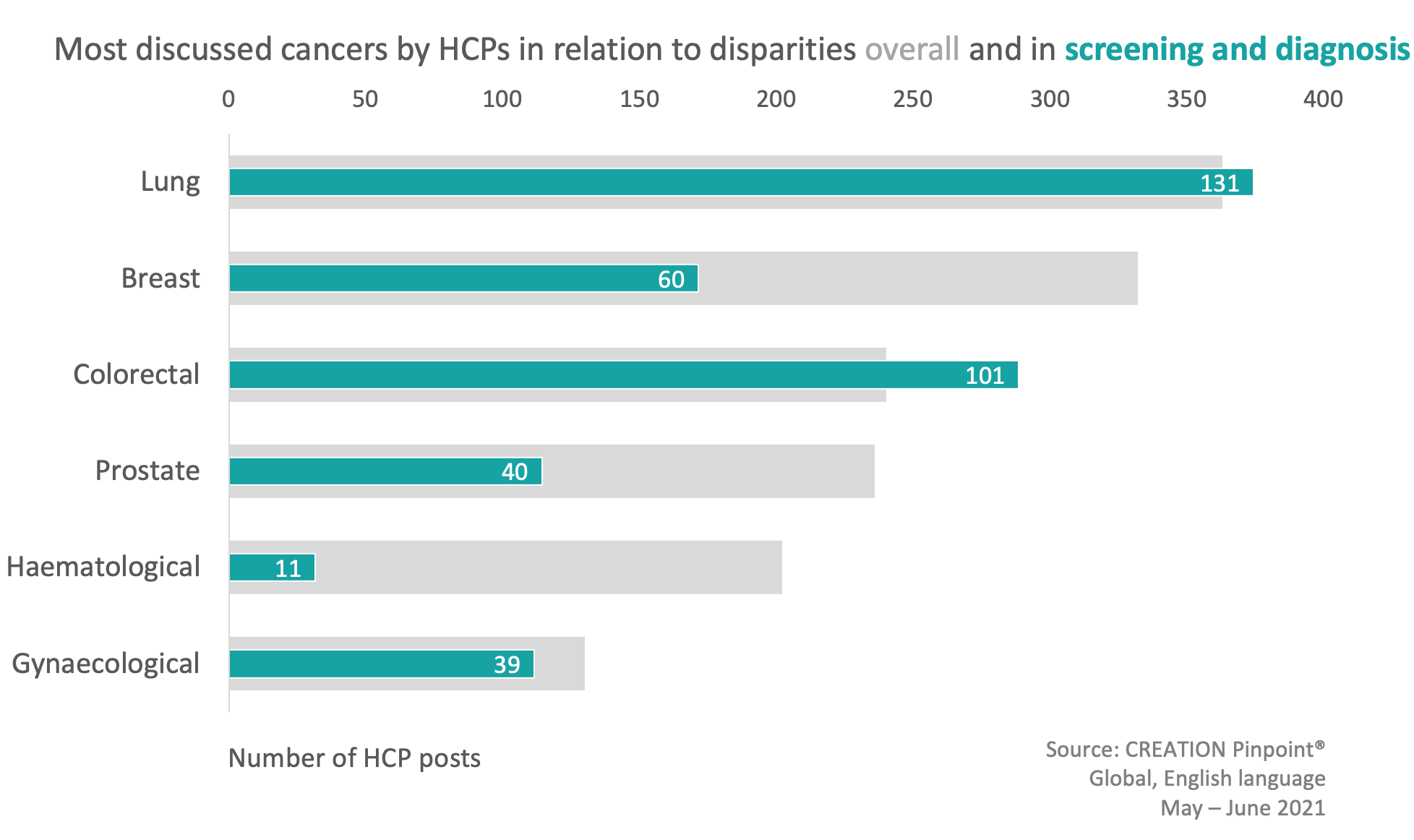
HCPs were able to circulate data giving evidence to specific areas of imbalance in cancer care. One such example is Dr Loretta Erhunmwunsee, a thoracic surgeon in California, who led a review on racial and socioeconomic disparities in lung cancer screening. The study identified consequences including higher mortality rates among disadvantaged individuals.

https://twitter.com/LorettaEMD/status/1396859433406267393
Congress season comes with a myriad of new product approvals and expansions, with no exception in the lung cancer landscape. Upon the approval of Amgen’s sotorasib (Lumakras), HCPs took the opportunity to highlight the need for all patients to receive next-generation sequencing (NGS) at diagnosis to identify targets required for personalised treatment. While new pharmaceutical products are being continually innovated and approved, online reactions bring to the forefront the reality that there remains to be patients who are unable to access these lifesaving drugs.
 https://twitter.com/RamalingamMD/status/1398958015395491847
https://twitter.com/RamalingamMD/status/1398958015395491847
Clinical Trial Enrollment
Aside from testing to pinpoint patients suited to targeted therapies, HCPs discussed the need for more representation in clinical trials. Diversity in trial participants is necessary to determine the safety and efficacy of drugs in different groups as these can be affected by age, gender, ethnicity, weight and even nationality. Data shared by Dr Toni Choueiri, as presented at #ASCO21, showed that black patients were significantly less likely to be treated in clinical trials.
 https://twitter.com/DrChoueiri/status/1400888181956952065
https://twitter.com/DrChoueiri/status/1400888181956952065
Further, Dr Shaalan Beg, posted an infographic detailing the root of this problem originating in an underrepresentation of black physicians in cancer care. ASCO’s snapshot showed that while comprising 13.4% of the US population, only 3% of oncologists are black. Another oncologist viewing these statistics said this was an “issue that we all must recognise and try to address”.
 https://twitter.com/ShaalanBeg/status/1395118132818284549
https://twitter.com/ShaalanBeg/status/1395118132818284549
Patient Experience
Social media is often home to conversations between HCPs and patient advocates, as well as a place where physicians can anonymously share patient stories, publicising successes and disappointments alike. During the virtual event, various patient advocates offered their viewpoints, including Dr Jacqueline Smith who is a melanoma survivor. Her session was posted by the likes of thoracic oncologist Devika Das, MD who called out stereotyping around skin cancer risk for those with darker skin.
 https://twitter.com/DevikaDasMD/status/1401213174611955712
https://twitter.com/DevikaDasMD/status/1401213174611955712
Oftentimes, HCPs are a crucial advocate for their patients, no less Mark Lewis, MD who uses his platform to call out barriers patients face at the hand of insurance companies. This post alone received considerable engagement and responses from other HCPs who had experienced similar events when seeking coverage for their patients.
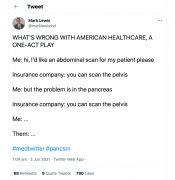 https://twitter.com/marklewismd/status/1400241842738798592
https://twitter.com/marklewismd/status/1400241842738798592
Moving Forward
ASCO 2021 and beyond has advanced discourse about inequity in cancer care. From race and nationality to gender and sexual orientation, new data and lived experience has revealed the extent of these issues, and even how they have been exacerbated by the COVID-19 pandemic.
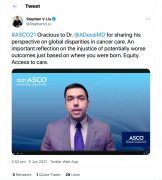 https://twitter.com/StephenVLiu/status/1401220516535582722
https://twitter.com/StephenVLiu/status/1401220516535582722
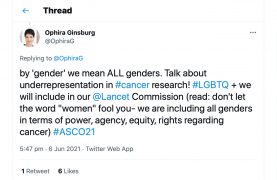 https://twitter.com/OphiraG/status/1401581593525899277
https://twitter.com/OphiraG/status/1401581593525899277
In terms of changing practice, HCPs drew attention to (sometimes unconscious) biases that are present throughout many patients’ experiences. Raising awareness to challenge such biases and educating healthcare providers to avoid inequitable conduct have been cited as steps to better circumstances from the source.
 https://twitter.com/drteplinsky/status/1401716368257564672
https://twitter.com/drteplinsky/status/1401716368257564672
Ultimately, this is an ongoing conversation and more than HCPs challenging their own practice, additional advancement should be expected at higher levels, from medical institutions, schools, and pharmaceutical and insurance companies. Nevertheless, the present discourse is reason to have hope for a brighter and more equitable future in cancer care, as well as to celebrate the strides already made.
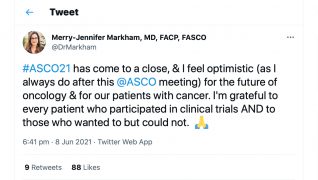 https://twitter.com/DrMarkham/status/1402320001537695744
https://twitter.com/DrMarkham/status/1402320001537695744
To understand the real-time unprompted views and opinions of healthcare professionals in any therapy area or health topic around the globe please get in touch, we’d love to help.
About the author
Mary Kangley, Senior Insights Analyst, CREATION.co. Mary is passionate about telling stories with data from online healthcare conversations. Her work is guided by a background in human and cyber-psychology providing a curiosity to understand #WhatHCPsThink.












