Spotlight on... breast cancer

To coincide with Breast Cancer Awareness Month (throughout October), Jackie Harris, Clinical Nurse Specialist at Breast Cancer Care provides an overview of breast cancer, including risk factors, breast awareness and treatments.
Breast Cancer Awareness Month takes place every October to promote the importance of breast awareness and highlight the issues facing people affected by breast cancer.
What is breast cancer?
There are several types of breast cancer; it is not one single disease. Breast cancer starts when cells in the breast begin to divide and grow in an abnormal way and it can be diagnosed at different stages of development and can grow at different rates.1
Breast cancer is the most common cancer in the UK. Rarely, it can be diagnosed in men. Around 55,000 people are diagnosed with breast cancer in the UK each year and of these about 400 are men.1
Secondary (advanced) breast cancer occurs when breast cancer cells spread from the primary cancer in the breast to another distant part of the body via the bloodstream or lymphatic system. A diagnosis of advanced disease means that the cancer cannot be cured, although it can be treated and controlled, sometimes for years. There are around 36,000 people currently living with secondary breast cancer in the UK.
Who is at risk?
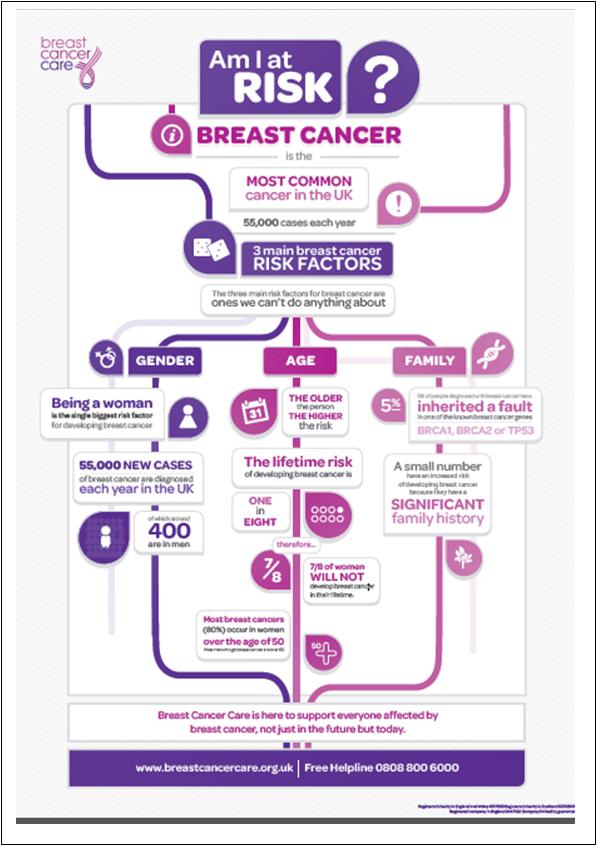
After gender (being female), age is the strongest risk factor for developing breast cancer – the older the person, the higher the risk. Over 80% of breast cancers occur in women over the age of 50.2
"After gender (being female), age is the strongest risk factor for developing breast cancer..."
Most cases of breast cancer happen by chance, though for a few, having a significant family history of the disease means that their risk is increased. About 5% of all breast cancers are caused by inheriting an altered gene, the two genes most commonly linked to hereditary breast cancer are BRCA1 and BRCA2.3 Anyone worried about family history of breast cancer and increased risk should speak to their GP.
Figure 1: A poster showing the factors that increase the risk of breast cancer
What are the symptoms to look out for?
There's no right or wrong way to check your breasts. Whatever your age, size or shape the most important thing to do is look at and feel your breasts regularly to get to know what's normal for you to help you notice any unusual changes.
It's important to check all parts of your breast, including under your arms and up to your collarbone.
You should look for:
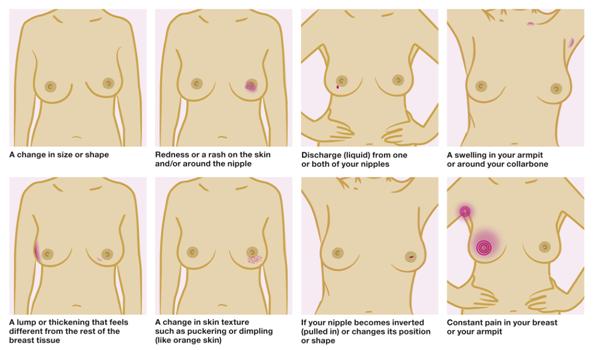
• any changes in skin texture such as puckering or dimpling, redness or a rash
• a change in the position or shape of your nipple
• a change in the size or shape of your breasts
• any lumps or thickening
• any discharge from your nipples
• constant pain or swelling in your breast or armpit
Figure 2: Diagram to show the eight signs and symptoms of breast cancer
Most changes won't turn out to be breast cancer, but don't be scared of talking to your GP or delay going, as the sooner a diagnosis is confirmed, the more effective treatment may be.
"There's no right or wrong way to check your breasts."
In the UK, women between the ages of 50 and 70 are invited for a mammogram (an x-ray examination of the breasts) every three years as part of a national breast cancer screening programme. It may help to detect breast cancer before there are any signs or symptoms. In England, this age range is being extended to 47–73 by the end of 2016.
What treatment is available?
Earlier detection and better treatments mean that survival rates after a diagnosis of breast cancer are improving; more than 8 out of 10 people survive breast cancer beyond five years.4 People can have different treatments, depending on what will work best for them.
If someone is diagnosed with breast cancer, their specialist team will discuss treatment options and their possible side effects with them. Many different factors will be considered when working out the best treatment for each person, including the type of breast cancer, their age and general health. Treatment may involve surgery, chemotherapy, radiotherapy, hormone therapy or targeted therapy, either given alone or in any combination or order.
"Earlier detection and better treatments mean that survival rates after a diagnosis of breast cancer are improving..."
What is the future?
More than half a million people are alive today in the UK after a diagnosis of breast cancer.5 The impact of breast cancer on people's lives doesn't stop when treatment ends. Preparing for life after treatment is an important time, for example adjusting to a 'new normal', whether it is managing ongoing side effects of treatment, considering a return to work or coping with the psychological impact. As more people are diagnosed and people are living longer with the disease, demand for information and support is growing and standards of care need to be improved.
For healthcare professionals, it's becoming increasingly important to address their patients' ongoing practical and psychological needs, tailor care to the individual, and know where to direct them for extra support.
References
1. The 55,000 figure is sourced from CRUK, refers to data from 2010 and is made up of 49,564 cases in women, 397 cases in men, and 4,647 cases of non-invasive breast cancer (DCIS). Incidence statistics for the nations does not include DCIS. www.cancerresearchuk.org/cancer-info/cancerstats/types/breast/incidence
2. These figures are sourced from CRUK, refer to data from 2010 and only apply to invasive breast cancer (doesn't include DCIS) www.cancerresearchuk.org/cancer-info/cancerstats/types/breast/incidence/#males
3. National Institute for Health and Care Excellence (NICE) Familial breast cancer clinical guideline June 2013
4. These figures are sourced from CRUK, refer to data from 2005-2009 and only apply to invasive breast cancer (doesn't include DCIS) http://info.cancerresearchuk.org/cancerstats/types/breast/incidence/#prev
5. The half a million figure is taken from Maddams J et al (2009) Cancer prevalence in the United Kingdom: estimates for2008, British Journal of Cancer. 101, pp 541-547
About the author:
Jackie Harris is a Clinical Nurse Specialist at Breast Cancer Care and has been working there for 11 years. Jackie has a remit and expertise in breast health, benign breast conditions and family history and has developed patient information and support services within these areas as well as lecturing to healthcare professionals.
Breast Cancer Care is the only specialist breast cancer support charity working throughout the UK. We were founded in 1973 by Betty Westgate, who was herself diagnosed with breast cancer. In the ensuing forty years we have supported millions of women and their families through our face-to-face, phone and online services. We also provide training, support and networking opportunities to specialist breast cancer nurses, and Breast Cancer Care publications are used by the majority of breast cancer units throughout the UK. We campaign for better support and care and promote the importance of early detection, involving people with breast cancer in all that we do.
Web: www.breastcancercare.org.uk
Free, confidential helpline: 0808 800 6000
How can we further support patients with breast cancer?