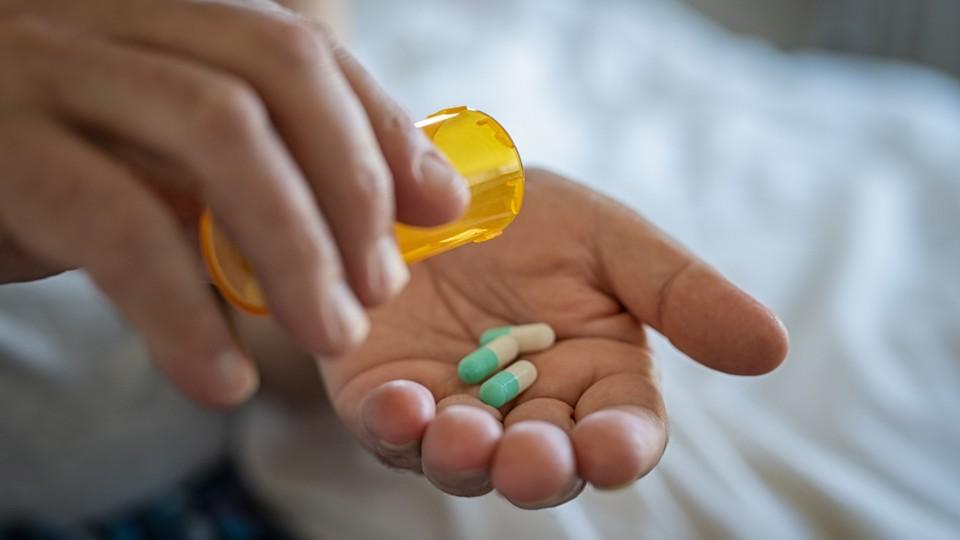
Medication adherence: how to ensure patients are not left behind
Poor medication adherence is both a costly issue for pharma manufacturers – with some estimating a loss of $600 billion each year – and a deadly issue for patients, with more than 100k preventable deaths estimated from patients not taking medications correctly, or at all. Tara Herington explores why medication non-adherence is a complex issue.
Communication is ever evolving and comes with distinct challenges for the pharma industry. The more complicated a medication or therapy, the more need there is for better communication with a patient. Do patients understand how often to take a treatment? Is there travel involved for an infusion or therapy? A specialist to see? Are there HCP concerns that require a medical information hotline?
More importantly, is the patient getting the message when they need it?
Understanding how and when patients would like to be communicated with is about more than just the latest social media channel or certain hours in the day. It comes down to not only personal preference but also a patient’s upbringing and generation. For example, older patients may expect a phone call before beginning treatment, while millennials will postpone treatment if a phone call is a requirement.
More so, research continually shows while the younger generations focus on digital technology, it is not all equal. Some may prefer texts over long emails or vice versa. There is also the question of whether the patients are managing their medicines themselves or if they are being managed by a caregiver. The average age of a caregiver sits at 49 years old, which would make them mainly Generation X – a generation that prefers short emails for communication. But maybe you know a drug is for the parents of small children? Or an early onset disease that would make caregiving children younger?
This focus on who is getting the message leads to another vital part of preferred communication with patients: the actual messaging.
Patients don’t begin every medication the same way. The pharma manufacturer needs to know if a patient is on their first therapy or fifth – and because of this, how will they respond to messaging? Do they delay treatment because they are in denial? Do they delay treatment because after four other therapies they are tired? Those examples require the pharma industry to meet the patients at different areas.
All of this proves that the best way to communicate with patients and caregivers is a personalized approach. After all, the more personalised medications become, the more personalised the communication efforts should be as well.
Understanding the cost barrier
There is plenty of research that showcases cost as a primary reason patients never start a medication.
However, it’s not enough for pharma manufacturers to assume that it is only the financial hardship facing a patient and deliver programmes just for that. The cost barrier may also refer to financial distress of patients in general, which is exacerbated by not knowing how much a drug costs when it is prescribed. This cause of patient stress and medication non-adherence has long been a problem in the healthcare industry.
According to a survey by Cardinal Health Specialty Solutions, socioeconomic factors of cancer patients are largely invisible to doctors who spend, on average, just 10 minutes with each patient. So, how, without being in the room, can pharma ensure both doctors and patients have better insight into the many patients they see on a daily basis? Especially when it could affect their health more?
COVID has laid the groundwork for more healthcare information to be more easily shared online, and the continued focus on AI and machine learning in our field may be the solution to allow doctors to focus on patients and pharma to analyse the data of all patients and continue to develop solutions.
Similarly, as the industry shifts towards personalisation, payers often scrutinise high-cost, specialised prescriptions more closely. Yet, this scrutiny reveals the need for faster, more efficient approval processes within fragmented health insurance systems. With a better focus on electronic benefits investigation (eBV) and electronic prior authorisation (ePA), pharma can help patients get on drugs faster, and help them feel more secure in their own financial situation, while doctor’s offices can feel more confident in knowing their patients can quickly access the medications they prescribe.
Examining adherence challenges with technology
Just as research shows that cost is the main factor for medication non-adherence, other research shows it’s not the only reason. And while healthcare providers and pharmacists may be able to list off plenty of reasons why a patient stopped a medication (side effects, feeling better, depression/anxiety, regarding the need for the medication, etc.) often the pharma manufacturers don’t get these answers. And because of this, they may be unable to develop the materials, training or programs to help current or future patients.
Enter technology.
This information can then be used to develop a better medical information programme for doctors/patients or to better understand patient hardships during certain time periods (like COVID), instead of simply leaving the concerns for the patient and doctor to work through among themselves.
There is much the pharma industry can do to ensure patients are not forgotten about when it comes to medication adherence. As healthcare technology continues to rapidly develop post-COVID, I’m excited to be see how the industry will embrace it.
About the author
Tara Herington is vice president at Cardinal Health Sonexus Access and Patient Support. She has more than 25 years of experience working in healthcare. In 2021, Tara was honoured as a Transformation Leader by PM360 in the PM360 Elite 100.