Gaps in breast cancer care in Europe and the importance of genomic testing
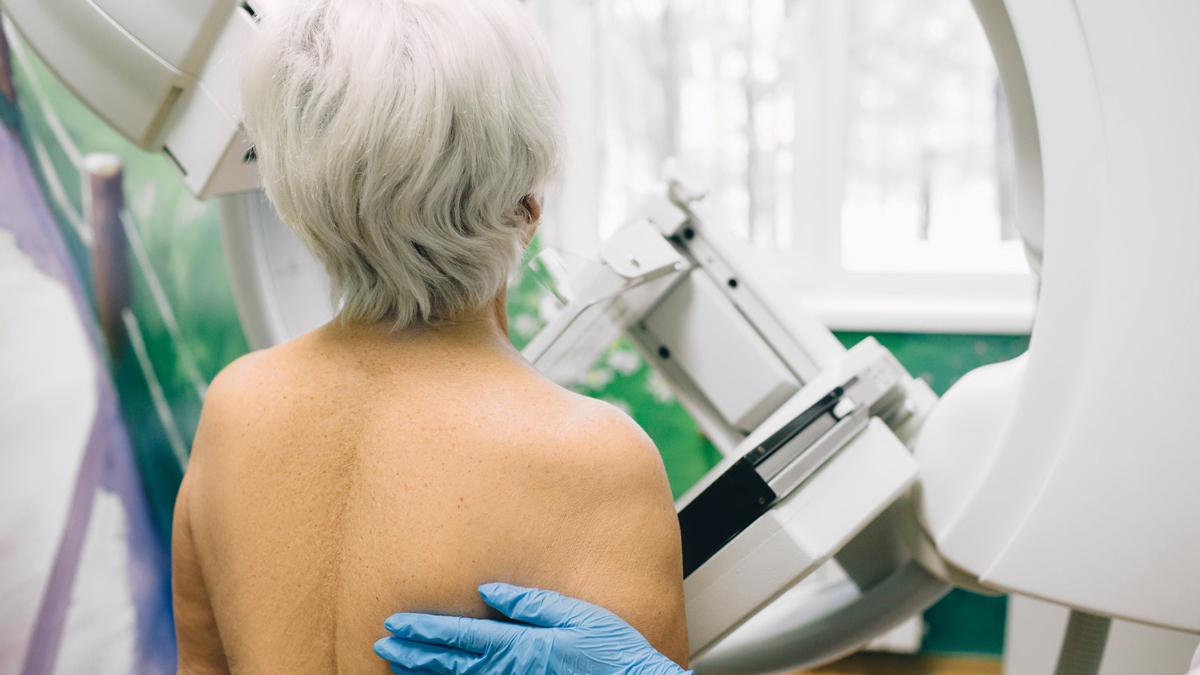
Breast cancer places a pressing burden on patients, physicians, and healthcare systems. Thankfully, breast cancer mortality decreased over the last five years in most European countries as a result of earlier detection through screening and treatment advances, including the growing role of precision medicine. However, as the leading cause of cancer death in women across Europe, more can be done to further improve breast cancer outcomes and save lives.
Two experts discussed their perspectives on precision medicine and the value of genomic testing to improve patient outcomes and how it can aid in closing gaps in breast cancer care in Europe. Antonella Cardone is chief executive officer at Cancer Patients Europe (CPE), a pan-European pan-cancer patient association, and Steven Bellamy is chief medical officer, international, at Exact Sciences, a global provider of cancer screening and diagnostic tests.
The current landscape for genomic testing in Europe
“There is a severe lack of awareness surrounding genomic testing in breast cancer in Europe, particularly in the patient community,” Cardone stated. “Patient groups have been aware of this for quite a few years, but we wanted to find out a little bit more about why this is the case.” This curiosity was the driving force behind a patient survey recently conducted by CPE, with the support of Exact Sciences, that showed significant gaps related to patient education and doctor-to-patient communication.
“Our understanding of breast cancer has evolved exponentially over the years, and it is now commonly understood that each person living with cancer is unique and no two cancer patients, or their tumours, are alike,” said Bellamy. “This is where genomic testing comes in.”
Genomic testing is a process that allows eligible patients the opportunity to potentially benefit from precision medicine, tailoring treatment plans to a patient’s individual cancer. In early-stage breast cancer, it can help in some treatment decisions, including whether patients are likely to benefit from adjuvant chemotherapy, sparing many women from this treatment and the associated side effects if they don’t need it.
The value of precision medicine
Genomic testing is one of the most important tools of precision medicine, which is a form of medicine that uses information about a person’s own genes or proteins to prevent, diagnose, or treat disease. “The benefit of precision medicine is in the name: it’s precise. Precision medicine tools provide specific information about a person’s tumour so that treatment plans can be tailored,” said Bellamy. “This is a major change from the one-size-fits-all treatment and prevention approach traditionally used and can lead to improved patient outcomes, as well as benefits for the healthcare systems.”
Cardone added that, “despite such utility from genomic testing and precision medicine, our survey demonstrated that 63% of breast cancer patients had not heard about genomic testing in cancer and only 25% of eligible patients living with breast cancer have taken a genomic test.”
Uncovering the truths in cancer care
This survey was a part of the wider ‘my Cancer my Concern (myC)’ initiative, set up by CPE with the aim to raise awareness of the benefits and value of genomic testing in cancer, educate patients, policymakers, and healthcare professionals, and improve accessibility to genomic testing across Europe. The project supports CPE’s broader goal of improving the management of cancer for patients and the survey was carried out as the first step of the myC initiative to better understand the level of patient knowledge about genomic testing.
Completed by a total of 1,383 respondents in Spain, Italy, France, Germany, and the UK, the survey revealed some uncomfortable truths about how breast cancer is managed across Europe, including that 78% or four out of five breast cancer patients eligible for genomic testing were not told they were eligible. “The results highlighted a critical need to increase efforts surrounding patient education, as well as doctor-to-patient communication,” noted Bellamy.
Other results exposed that 55% of cancer patients did not know the difference between genetic and genomic testing, and 84% of eligible patients did not feel as though they had enough information to make an informed decision on whether to take a genomic test. “These figures confirm what patient organisations have observed anecdotally through their work: that work needs to be done to increase awareness of the value of genomic testing in breast cancer to ensure patients have access to optimal care across Europe,” Cardone commented.
A path to better patient outcomes
With this knowledge, CPE and Exact Sciences have highlighted that the gap in genomic testing awareness must be tackled and improvements need to be made in the shared decision-making process between a patient and their doctor. Bellamy commented that this begins with industry, and that “as a provider of cancer diagnostics, as Exact Sciences is, for example, we promote scientific exchange and education initiatives on the value of genomic testing among physicians, and we partner with organisations such as CPE in order to raise awareness in the patient community.”
About the interviewees
 Antonella Cardone is the CEO of Cancer Patients Europe (CPE), the pan-European and all-cancer types patient association. She is the patient advocacy expert and advisor to the Board of Pancreatic Cancer Europe (PCE), the European multi-stakeholder platform of groups of physicians and patients, politicians, journalists, academia, and industry on pancreatic cancer. Cardone is the former director of the European Cancer Patient Coalition (ECPC).
Antonella Cardone is the CEO of Cancer Patients Europe (CPE), the pan-European and all-cancer types patient association. She is the patient advocacy expert and advisor to the Board of Pancreatic Cancer Europe (PCE), the European multi-stakeholder platform of groups of physicians and patients, politicians, journalists, academia, and industry on pancreatic cancer. Cardone is the former director of the European Cancer Patient Coalition (ECPC).
 Steven Bellamy currently serves as chief medical officer, international, at Exact Sciences. Over the past 20 years, Bellamy has held many positions across the health and life sciences industry and he has deep medical and clinical affairs expertise, with extensive experience in oncology, rare diseases, and cardiovascular diseases.
Steven Bellamy currently serves as chief medical officer, international, at Exact Sciences. Over the past 20 years, Bellamy has held many positions across the health and life sciences industry and he has deep medical and clinical affairs expertise, with extensive experience in oncology, rare diseases, and cardiovascular diseases.











