FDA gives breakthrough status to Biofourmis' heart failure DTx
A digital therapeutic for patients with heart failure has been awarded breakthrough device status by the FDA – said by its developer Biofourmis to be the first time the US regulator has given this designation for this type of product.
Boston-based Biofourmis claimed the accolade for its BiovitalsHF prescription digital therapeutic (DTx), which is used to make sure that patients who have heart failure with reduce ejection fraction (HFrEF) get the right drug treatment in accordance with clinical guidelines.
Biofourmis' chief executive and founder Kuldeep Singh Rajput said it is a significant step for the advancement of the digital therapeutic category, as well as for patients with heart failure.
Breakthrough device designation can speed up the development of new medical devices, making them available to patients sooner – a key consideration for Biofourmis as BiovitalsHF is currently under review by the US regulator.
The framework has been available in the US since 2018, and is analogous to the breakthrough designation that can be awarded to drug products that promise to provide a step forward in the treatment of diseases.
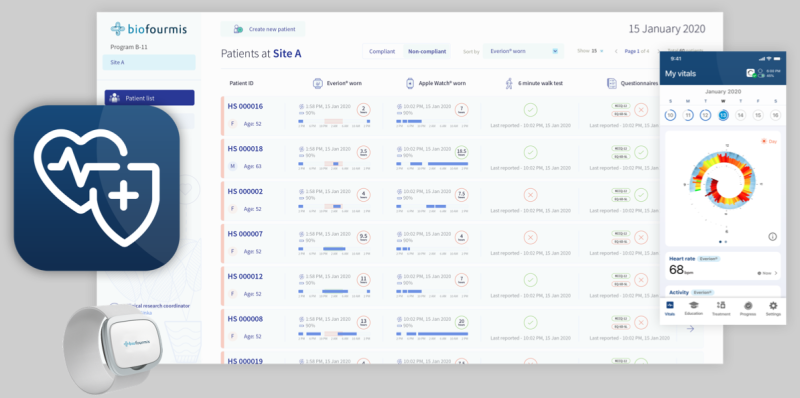
BiovitalsHF uses software algorithms and wearable sensors to help direct drug treatment for HFrEF, encourage patients' adherence to treatment, and monitor their progress.
It has been designed to follow guideline-directed medical therapy (GDMT), a strategy of gradually phasing in different medications including ACE inhibitors, angiotensin 2 receptor antagonists and beta blockers to try to improve left ventricular ejection fraction – the amount of blood pumped out with each beat of the heart.
GDMT has been shown to reduce morbidity and mortality in HFrEF patients but is still not applied to all patients. Biofourmis says it has clinical data showing that BiovitalsHF can improve adherence to GDMT, reduced biomarkers of heart failure, and improve health status scores in HFrEF patients.
"BiovitalsHF gets patients on the right therapies faster, which studies have shown helps save lives, prevents emergency department visits and hospital admissions, and enables patients to have a better quality of life," according to Maulik Majmudar, Biofourmis' chief medical officer.
The company says there are around 6.2 million people in the US living with heart failure, and the estimated annual cost of treating the condition is expected to reach $70 billion a year by 2030.
It is estimated that less than 1% of the heart failure patients are on optimal doses of heart failure medication, and that is thought to contribute to poor treatment outcomes – around one in four patients are re-hospitalised within 30-days of discharge.











