Your health, yourself: Claude’s case of compliance

In the third part of this series by Ogilvy CommonHealth Worldwide on the quantified-self movement, we meet Claude who is struggling to take his hypertension medication.
(Continued from "Your health, yourself: Marta's nutrition mission")
Over the course of this series you will be introduced to Thiery, Marta, Claude, Dana and Harry – each of whom (like most of us) have specific health concerns to deal with and / or wellness goals to reach. As both consumers and patients today, they have access to a wide range of personalised technology that promises to smooth their path to wellbeing. But whilst in theory these individualised offerings are more effective than traditional approaches, in reality success is far from guaranteed. It seems that even though health information is readily available at the touch of the button or a swipe of the finger, it is rarely packaged in a way that is truly relevant and meaningful to us as consumers.
Meet Claude. He's a 43-year-old family man who has recently been diagnosed with hypertension. His physician has prescribed him a broad range of medications (in fact it seems to Claude that there is a new one everyday), accompanied by strict instructions on the importance of taking them daily. Both his doctor and his wife (the latter via a lot of Googling) have forewarned him of the unpleasant consequences his disease could bring. At the bottom sits a myriad of minor complications and time-consuming visits to the clinician, in the middle follows a range of irreversible impairments from cardiac events and right at the top: DEATH. By all accounts Claude's got a lot of good reasons to adhere – and he does, but only sometimes.
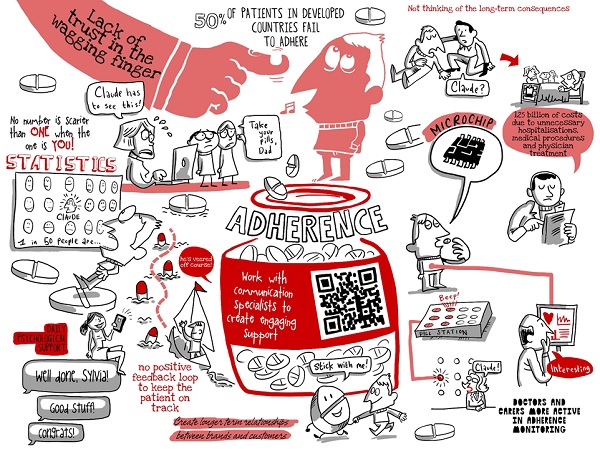
So why don't death, decline and inconvenience weigh more heavily on Claude's mind? It may seem nonsensical to an observer, but the reality is that Claude's attitude is a common one – only 50% of patients in developed countries adhere to their medications as prescribed1. It is estimated that each year in the EU alone, mis-dosing and non-adherence results in 194,500 otherwise preventable deaths and €125 billion of costs due to unnecessary hospitalisations, medical procedures and physician treatments2. And all of this is without even considering the impact of poor health on productivity and quality of life. Furthermore, Claude's hypertension is only one of a myriad of diseases that suffer from poor adherence. In diabetes, good glycaemic control is associated with reduced resource utilisation; however, 43% of patients don't achieve adequate control and insufficient medication is a key reason for this3,4. Likewise for those with schizophrenia, risk of relapse is 3.7 times greater if they are non-adherent – yet this is the case for over 50% of patients their first year out of hospital5. Sobering statistics. So again we have to ask, why is this the case? Surely our health is our most valuable asset. Well the fact is that many patients, even when faced with the wagging finger of a clinician, fail to connect the consequences of their inaction to the serious, and often inevitable, health risks of non-adherence. The reasons for this are complex. Adherence is strongly influenced by the environment in which people live, as well as how healthcare systems and practitioners deliver care. It is also intrinsically linked to an individual's perception of illness, their level of self-management, confidence and motivation and preconceptions about the outcome of treatment1. So maybe it is that Claude lacks trust in that wagging clinician finger, especially if that finger continues to push an ever increasing range of medications in his direction. Or it might be that unlike much of today's world, there is no independent positive feedback loop to help him stay on track. Side effects, whilst minor, are real and present; long-term consequences are mere probabilities. For Claude, adherence brings no instant reward nor immediate punishment.
So how can we help Claude face reality? To date, two main approaches have been taken to deal with non-compliant patients like Claude. The first, education, strives to improve knowledge and awareness of risks but can be costly, time- consuming and often ineffective. The second – the simplification of treatment regimens – aims to alter the dosage frequency or mode of administration of certain drugs, most notably statins. Some success has been enjoyed in both areas but two things are still clear: simplifying a dosing regimen is unlikely to affect a person who does not believe that the therapy will improve their health; and knowledge alone is not enough to ensure good adherence habits. On top of this, healthcare systems tend to see adherence from the perspective of the overall population, which means that the impact on individuals is lost among the statistics. Yet no number is scarier than One, when the 'One' being referenced is you. So providing more personal health information to patients like Claude may be the best way to tackle the problem of non-adherence.
There are already a number of successful examples utilising this approach in the marketplace, suggesting that such a strategy has potential. In the spheres of smoking, weight loss and diabetes for example, daily psychological support can be provided for extensive periods online, with patients receiving individual progress reports and goal-orientated messaging via interactive websites and SMS. Furthermore, such programmes can address 'non-compliance' with specifically targeted customised messages, and offer follow-up support for months or even years after the health goals have been reached – two methods that behaviour change studies have found to be particularly effective6.
The digital technology behind these approaches allows patients to be reached at any time of the day, wherever they may be – putting medication in the forefront of minds and naturally building adherence into lives like never before.
But guess what? Once again, just as we saw in nutrition and fitness, these new methods prove to be most effective amongst patients who are already reasonably well motivated and 'digitally-savvy'. What about those people who simply can't remember to take their medicine, or don't want to? For these patients, a different approach is being explored that allows doctors and carers to take a more active role in adherence monitoring. One example of these new 'smart technologies' has been designed by SentiCare® to let a designated care advisor know when a patient has forgotten to take their medicine or otherwise veers from their prescription guidance. The technology revolves around an intelligent 'PillStation', which scans pill containers whenever the lid is closed.
"...providing more personal health information to patients like Claude may be the best way to tackle the problem of non-adherence."
Some are taking this smart technology even further. The latest methods being tested actually put microchips into medicines, allowing HCPs to track the treatment as it passes through the body, thereby monitoring how and when it is delivered to the individual. In August 2012, the US FDA approved the first such pill for testing and many think that this type of personalisation holds a lot of potential for the future. In markets where patients are reimbursed for prescriptions, microchip tracking could be linked to economic incentives to ensure full treatment compliance.
What lies ahead for patients like Claude? There is an obvious opportunity for pharmaceutical companies and healthcare providers to strengthen their products' value propositions by providing programmes which support optimal adherence. Patient education, ongoing patient support, training for personal and comprehensive communication strategies can all help patients like Claude stay on track when they most need it. And the patient is not the only beneficiary. Adherence programmes can be a great way to create long-term relationships between brands and consumers, enhancing corporate reputations and encouraging loyalty.
In order to create an environment that supports optimal adherence, it will be essential for the industry to work with communication specialists in order to truly understand the distinct needs of different audiences. Input from multiple stakeholders will be needed to develop messages and tactics that are effective in influencing behaviour. The urgency in realising this opportunity will become increasingly apparent as non-traditional healthcare players, routed in big data, strip funding from medications and emphasise the non-pharma aspects of treatment regimens. So Claude, it's time to take your medicine!
Health highlights:
Non-adherence is a serious problem for the healthcare industry, costing lives and money.
Personalised approaches to compliance have the potential to improve individual adherence behaviour.
Do:
• Work closely with expert communicators and multiple stakeholders to create truly engaging patient support programmes
• Embrace new technologies to support those unable or unwilling to take responsibility for their own treatment compliance
Don't:
• Treat adherence from a total population perspective – solutions should be tailored to the individual.
References
1. World Health Organization. Adherence to long-term therapies: evidence for action. Available at: http://www.who.int/chp/knowledge/publications/adherence_report/en/ (Last accessed May 2013).
2. World Health Organization. Fifty-fifth World Health Assembly. Third report of Comittee A. Available at: http://apps.who.int/gb/archive/pdf_files/WHA55/ea5552.pdf (Last accessed May 2013).
3. Briesacher BA, et al. Comparison of drug adherence rates among patients with seven different medical conditions. Pharmacotherapy 2008;28:437–43.
4. Cutler DM, Everett W. Thinking outside the pillbox. N Engl J Med 2010;362:1553–5.
5. Fenton WS, et al. Determinants of medication compliance in schizophrenia: empirical and clinical findings. Schizophr Bull 1997;23:637–51.
6. Krueger KP, et al. Improving adherence and persistence: a review and assessment of interventions of steps towards a national adherence initiative. J Am Pharm Assoc 2003;43:668–79.
The next article in this series will be published next week.
Other articles in this series:-
Your health, yourself: Thiery's technotraining
Your health, yourself: Marta's nutrition mission
About the authors:
Carsten Edwards is Managing Partner, Ogilvy Healthworld Market Access, UK;
Jean-Marc Mosselmans is CEO, Ogilvy Healthworld France;
Michael Dumigan is Senior Global Planning Partner, Ogilvy Healthworld Strategy and Planning, UK
Closing thought: How can we support patients to understand the consequences of their non-adherence?











