Spotlight on...leprosy

Nicolette Dawson and Dr P. V. Ranganadha Rao
LEPRA and LEPRA India
This month’s spotlight on article looks at leprosy, which is a disease of the nerves and skin. Many people think leprosy is associated with poverty, but this is not strictly true. Nicolette and Dr Rao explain the treatments available and how pharma can better support patients.
What is Leprosy (Hansen’s Disease)?
Leprosy is mainly a disease of the nerves and skin, caused by bacteria called Mycobacterium Leprae or M.leprae. Leprosy is important mainly because of the damage it does to nerves. Nerve damage is the main disability people with leprosy develop, which can affect the cooler parts of the body e.g. eyes, nose, testes, fingers and toes.
Who is at risk?
One person is diagnosed with leprosy every two minutes. The problem in determining who is at risk is, we just don’t know.
We know that leprosy is spread from person to person, but we don’t know how. Most people with leprosy are not infectious and M.leprae multiply very slowly, which means that leprosy can have an incubation period of several years before signs start to appear. Most people are naturally immune to leprosy. Out of 100 people, if all were infected only around three would develop leprosy.
 ,
"One person is diagnosed with leprosy every two minutes."
 ,
Leprosy is often associated with poverty, but is not strictly a disease of the poor. It affects impoverished people to a much greater extent, because of their social and economic vulnerability. In India, which is home to more than half of new cases each year, the stigma attached to leprosy leads to loss of employment even before manual labour becomes more difficult due to disability, which often results from late or no treatment. It also leads to exclusion from society, causing physical and emotional distress.
What are the symptoms to look out for?
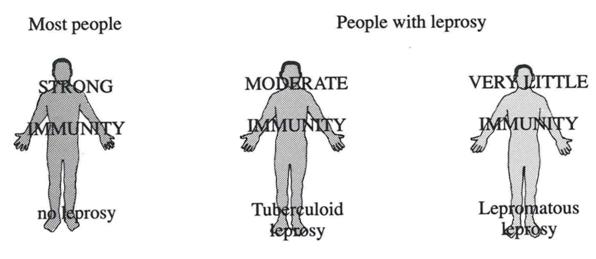
Different strengths of immunity give rise to different types of leprosy. Leprosy, in most of the cases, starts with ‘anaesthetic’ skin lesions, without pain and touch sensation.
Figure 1: Diagram from book: Leprosy for Field Staff, A Summers.
Where people have moderate immunity, their body can prevent the M.leprae from reaching large numbers and spreading throughout the body. They will have signs of leprosy in only a few parts of their body.
Where there is little immunity to leprosy, M.leprae will multiply freely and signs of leprosy will be found in many parts of the body, including the skin and in some cases, a person’s bones.
 ,
"...if diagnosed early and treated properly, leprosy should leave no lasting damage."
 ,
Nerve damage from leprosy affects the motor, sensory and autonomic fibres. Symptoms include some or a combination of: paralysis, pain, loss of sensation or anaesthesia in hands, feet, skin or cornea, the development of what is known as ‘leonine face’, loss of eyebrows and eyelashes, skin lesions.
What treatment is available?
Leprosy has been curable since the 1980’s, with a combination of drugs called multi-drug therapy available free to governments through the World Health Organisation (WHO), if diagnosed early and treated properly, leprosy should leave no lasting damage.
Treatment requires careful monitoring for compliance (patients can sometimes stop treatment too early), drug resistance, side effects and leprosy reactions (malaise, fever, pain, inflammation in the eyes, nerves and joints), which in themselves can speed up nerve damage and cause disability.
Despite this, leprosy continues to leave many people with permanent physical impairments, with more than three million people living with these today.
How can pharma best support patients with leprosy, and what needs to be done in the future?
Fighting leprosy today goes beyond the availability of a cure. Drugs alone do not work. Leprosy is a prime example here. The narrow focus imposed by the World Health Organization has had a negative impact on early detection of leprosy and funding for disability management.
 ,
"Fighting leprosy today goes beyond the availability of a cure. Drugs alone do not work."
 ,
Funders sometimes appear to be out of step regarding the emergent needs in the field. Their approach, focussing on the delivery of pills, is by its very nature running the unwanted risk of being simply too narrow in focus.
Yes, we need the drugs, but we also need funds for research, education, capacity building within government health structures and staff to prevent disability, as well as to manage the burden of disease for the millions of victims left behind.
In addition to this, we need to continue to support leprosy-affected people in finding a voice and accessing their rights to equal treatment and healthcare. LEPRA currently does this in India by supporting leprosy-affected people at community level to be represented at state level, in particular ‘SLAP’ which is the society for leprosy affected people.
Some previous 'Spotlight on...' articles:
 ,
 ,
About the authors:
Nicolette Dawson, communications officer
Nicolette Dawson is communications officer for LEPRA. She is responsible for communications and branding for LEPRA in the UK. This includes internal communications and fundraising support, media relations, website and social media engagement.
Nicolette has a background in marketing communications gained in a variety of industries from professional services to manufacturing. She has an honours degree majoring in Marketing and corporate strategy.
Dr P.V. Ranganadha Rao, Chief Executive
Dr P. V. Ranganadha Rao, Chief Executive of LEPRA India, has been appointed as International Medical Director for LEPRA Health in Action. His role will be to ensure the continued development of quality of care throughout the organisation. Dr Rao joined LEPRA India in 1989 as medical officer at LEPRA Hyderabad leprosy project (HYLEP) and in 2003 he was appointed as Chief Executive of LEPRA India.
Before joining LEPRA, Dr. Rao worked for two years as a medical officer in a Leprosy hospital supported by the German Leprosy Relief Association, and for 5 years in the Indian Army Medical Corps.
Dr Rao has 20 publications to his credit and has presented papers in international conferences covering Leprosy, TB, HIV / AIDS and tropical diseases like Lymphatic Filariasis. He also participated in the evaluation of Maldives leprosy eradication programme commissioned by SEARO, WHO.
How can pharma best support patients with leprosy?