How post-fracture care programmes such as fracture liaison services can bridge the treatment gap for osteoporosis
As society globally faces a growing elderly population, age-related conditions such as osteoporosis are coming to the forefront as critical issues. More emphasis needs to be placed on secondary fracture preventative services to reduce the burden of osteoporosis-related fractures, known as fragility fractures, on patients and healthcare systems.
With an ageing global population, osteoporosis is becoming a global epidemic and its prevalence is set to increase.
Osteoporosis currently affects around 200 million people globally, resulting in almost 9 million fragility fractures annually.
The World Health Organization (WHO) estimates that by 2050, the proportion of the world’s population over 60 years of age will be 22%, nearly double what it was in 2015, putting 2.1 billion people into the 60 and over age group and at risk for age-related diseases.
Worsening health in older members of the population generally has been linked with the deceleration of economic development. The reasons for this are numerous, but can be associated with a lower rate of employment for the working-age population, whose participation in the workforce is crowded out by family caregiving. In addition, there are specific and direct economic consequences of osteoporotic fractures that have been shown to exceed those for other conditions such as migraine, stroke, multiple sclerosis, and Parkinson’s disease.
Osteoporosis can cause fragility fractures that have a detrimental impact on the individual; for example, hip fractures have been shown to lead to poor health outcomes in terms of pain, loss of mobility and function, and increased mortality. A prior fracture is associated with an 86% increased risk of any fractures. To learn more, pharmaphorum spoke with Nico Reynders, Senior Vice President, Head of Bone Health Mission at UCB, and Masatoshi Morita, Head of Japan, Bone Health Mission at UCB, as they explained the work the company is doing in providing measures to encourage optimal care of those living with osteoporosis. Both explained this can be achieved through the utilisation of Fracture Liaison Services (FLSs), which is a multidisciplinary approach to reducing the risk of fractures in those living with osteoporosis.
The scale of the challenge
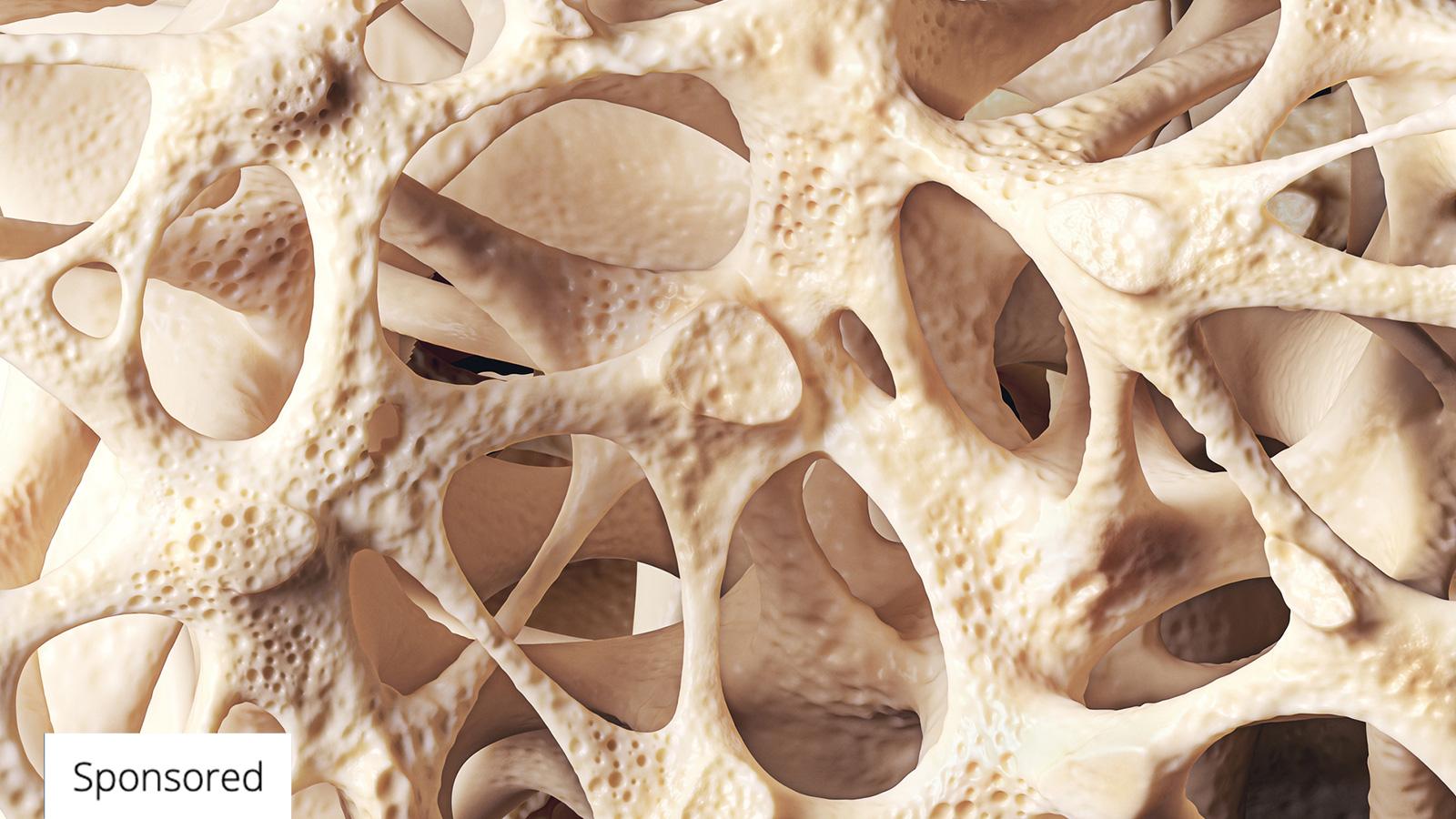
Osteoporosis occurs when more bone is broken down than is replaced by the body. Due to the condition, the outer shell of the bone becomes thinner, and the natural spacing inside the bone becomes larger. This leads to the bone becoming weaker and more fragile, resulting in fractures.
On an individual level, the burden of living with osteoporosis can be extremely difficult.
Reynders explained the challenges for those living with the disease: “After suffering a fragility fracture, such as a hip fracture, it can negatively impact quality of life. It can impede function, resulting in loss of independence and affecting one’s emotional well-being. Once you have suffered from an initial fracture, there is also a significantly higher risk of an additional fracture.”
Research has found that osteoporosis will cost the US $25 billion per year by 2025, with this figure rising to an estimated $95 billion by 2040 in direct medical costs, as well as indirect societal costs related to productivity losses and informal care. In Europe, the costs are similarly high, with estimates suggesting that the 4.3 million fragility fractures occurring annually cost the healthcare systems across the region in excess of €56 billion each year. Research indicates that the treatment gap – that is, patients who have experienced a fracture, but are not diagnosed with osteoporosis, leading to a lack of follow-up care and appropriate treatment – is increasing. In fact, it is estimated that 80% of those who experience a fragility fracture are not identified or treated with effective therapies. This results in a higher chance of further fragility fractures, which means more time spent by the patient in acute care and additional costs to the system.
Morita outlined how this can occur: “In Japan, with a hip fracture, the patient will likely spend two weeks at the acute phase for surgery. From there, they are moved to the rehabilitation hospital to recover their function. At the end of this phase, for the maintenance, they will typically return to the clinic or to a nursing home. During this journey, they can often change physicians and the appropriate information may not be shared to receive a diagnosis. Due to the limited number of osteoporosis specialists, the patient often may not see an expert in the area and learn the cause of the fractures, which is osteoporosis.”
As a result of this lengthy process, it can take many additional fractures for patients to be finally diagnosed accurately. More than this, Reynders added, “there are a number of other factors that can potentially delay the correct diagnosis. For instance, if a patient lives in a rural area, there are likely to be far fewer osteoporosis specialists in the disease area.”
Breaking the cycle
Ensuring that patients are able to get out of the cycle of experiencing fragility fractures requires effective management and adequate support, said Morita. However, he noted that this can be difficult to secure when care is disjointed. A means to help catch those patients falling through the net has been the development of coordinated post-fracture care services, such as Fracture Liaison Services (FLSs).
FLSs adopt a multidisciplinary approach to reduce subsequent fracture risk in patients with a recent fragility fracture. The service identifies patients that have been treated in hospital for a fracture, and then performs an assessment to determine whether they have osteoporosis and are at risk for subsequent fractures, allowing timely and effective intervention. The International Osteoporosis Foundation has stated that the implementation of FLSs is the most important action that can be taken to directly improve patient care and reduce the cost of fractures in healthcare systems. According to Morita, the multidisciplinary effort requires bringing together all aspects of care to focus on reducing the risk of subsequent fractures.
“This means a multidisciplinary effort, which not only involves the orthopaedic surgeon caring for the fracture, but also treatment for osteoporosis. This includes investigating the risk for a secondary fracture, beginning a course of treatment, and also complementing drug treatment with exercise and nutrition. We need to work collaboratively together with pharmacists, nurses, and physiotherapists for this to happen,” Morita explained. One of the barriers to greater adoption of FLSs is the initial cost. Though people living with osteoporosis and the fractures that occur are expensive to treat, working to join up services and provide FLSs means healthcare systems face upfront costs. For instance, if the services are not reimbursed, hospitals will have to support this financial burden, which may not be possible. “The linking of services within a hospital or care services may also be tricky depending on the country. Different healthcare systems will have varying structures, and a successful implementation of FLSs can be dependent on how advanced the existing framework is,” said Morita.
A case in point
In Japan, national and international organisations, supported by UCB and AMGEN, worked with healthcare professionals to discuss the issue of the fragility fracture care gap with healthcare policy makers. The dialogue between stakeholders looked at ways to successfully implement FLSs and to ensure that the services receive reimbursement for hip fracture. In order to create FLSs that would provide an immediate positive impact, the partners studied the implementation of the services in different countries, including the UK and New Zealand. As of 1st April 2022, the FLS reimbursement scheme was updated, providing better support to the estimated 200,000 people who suffer a hip fracture every year in Japan.
Morita relayed that, since this change, approximately 1,800 hospitals in the country have applied for the FLS reimbursement scheme. Morita also noted that the two core elements added to the updated scheme include surgery within 48 hours, and the evaluation/treatment for osteoporosis. Reynders stated: “The earlier people get on the right treatment, the higher the chances that the subsequent fracture risk is reduced. If you can potentially reduce multiple fractures to just one, that’s important for societal cost, but, more importantly, it’s a quality-of-life improvement for the individual.”
After proving the efficacy of FLSs through implementation in countries such as Japan, the next step will be to encourage their adoption and uptake in other countries. Reynders added: “Advocating for the global implementation of FLSs is an essential component of our approach to closing the care gap. However, exactly how FLSs integrate into existing healthcare systems will be very different from country-to-country. We aim to bring together the right partners in each country, implementing both top-down and bottom-up strategies to elevate secondary fracture prevention as a healthcare priority and highlight the critical role FLSs play.”
“From a bottom-up perspective, we focus on both quantity and quality – how to implement as many FLSs as possible, whilst ensuring the optimal standard of care for patients by gradually improving the quality of each FLS.”
“Lastly, we work closely with partners such as the Fragility Fracture Network and the International Osteoporosis Foundation, whose Capture the Fracture® programme now includes more than 833 FLSs worldwide. Partnering with both local and global organisations can help raise awareness. In the case of Japan, it was the best approach and brought us a step closer to ensuring that the first fracture a patient experiences is their last.” Reynders concluded.
About the Interviewees
 Nico Reynders, Senior Vice President, Head of Bone Health Mission at UCB
Nico Reynders, Senior Vice President, Head of Bone Health Mission at UCB
 Masatoshi Morita, Head of Japan Bone Health Mission at UCB
Masatoshi Morita, Head of Japan Bone Health Mission at UCB
About UCB

UCB, Brussels, Belgium is a global biopharmaceutical company focused on the discovery and development of innovative medicines and solutions to transform the lives of people living with severe diseases of the immune system or of the central nervous system. With more than 8,000 people operating in more than 40 countries, the company generated revenue of €5.3 billion in 2020. UCB is listed on Euronext Brussels (symbol: UCB).










