Need for non-melanoma skin cancer guideline never greater
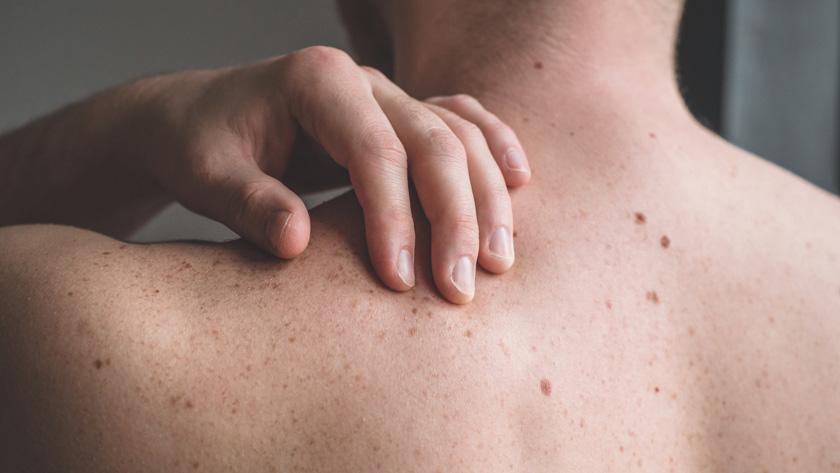
Non-melanoma skin cancer (NMSC) is the most common cancer in the UK, more than breast, bowel, and prostate cancer combined. Over the last decade, NMSC incidence rates have increased by more than 42% in the UK, and they’re predicted to reach almost 400,000 per year by 2025. However, while cases are continuing to rise, NMSC is significantly under-recognised and under-prioritised by national and local health systems, with widespread inconsistency in NMSC patient pathways.
To better understand the steps that can be taken to help improve outcomes for people living with NMSC, we conducted a survey of 95 skin cancer experts in the UK. Informed by their insights, and endorsed by Skin Cancer UK, we have identified clear challenges that patients face when seeking support and treatment for NMSC. We have also gained greater knowledge about what can be done to overcome these barriers.
There is no comprehensive, national clinical guideline for NMSC patients
While multiple guidelines exist, most are either outdated or do not focus on the full NMSC pathway. As a result, there are multiple inconsistent national and local care pathways throughout the UK, with some areas not having a pathway in place for patients at all. What are the implications?
Variations in definitions of NMSCs
There are variations in the definitions used to distinguish NMSCs. The two most common types of NMSC are basal cell carcinoma (BCC) and squamous cell carcinoma (SCC). The definitions to distinguish the two vary between different locally adopted guidelines: some use growth rates and lesion (abnormal tissue) size, whereas others do not provide any specific parameters. BCC has established definitions for advanced tumours, but no consistent clinical definition of advanced SCC exists. These inconsistencies are leading to delayed diagnoses and impacting the NMSC patient care pathway and options.
Inappropriate referrals and management of NMSC
Differences exist between which clinical team can and should be treating cases. NMSC patients with lower risk lesions should be referred to a local hospital skin cancer multidisciplinary team (LSMDT), which deals with less urgent cases, or a specialist hospital skin cancer multidisciplinary team (SSMDT) for cases that may require more intensive treatment. However, in practice, patients are sometimes referred to Head and Neck Specialists, as NMSC typically appears in these areas on the body. As such, access to appropriate treatment may be delayed.
When NMSC patients are seen by a Head and Neck Specialist, multidisciplinary teams (MDTs) should work together to provide the best possible care. This requires close contact between clinical teams and allied professionals, yet, existing guidelines do not often account for communication between them, and often lack contact details.
Differences in data collection
Accurate and reliable data collection is lacking on diagnosis, time to treatment, and patient experience. For NMSC data that is collected, there are huge variations in how it is recorded across different areas. England and Northern Ireland only register the first NMSC a patient is diagnosed with; in Scotland, all SCCs are recorded, but only the first BCC; and Wales does not publish its NMSC data. Without information, it is difficult for health bodies to effectively plan care and meet the growing demand for services.
The workforce crisis must be addressed to effectively implement national NMSC guidance
The effective implementation of a comprehensive, national clinical guideline requires a sufficiently resourced workforce. As things stand, shortages exist in all specialisms along the NMSC patient pathway. Furthermore, skin cancer is one of three cancers that comprise two thirds of the national COVID pandemic backlog in England. As a result, clinical teams are working through huge waiting lists, and NMSC patients are being diagnosed at more advanced stages of disease, due to later presentation.
Sanofi’s recommendations for improving the NMSC patient experience in the UK
In our report, The Non-Melanoma Skin Cancer Patient Pathway: Improving Patient Journeys and experience of Care, which summarises the survey findings in more detail, we published concrete recommendations for overcoming these challenges, and in turn, alleviating system pressures.
- National bodies across the UK must update and publish a comprehensive, national clinical guideline in NMSC.
97% (n=92/95) of skin cancer experts we surveyed agree that NICE should publish a specific national guideline on the referral and management of NMSC, with 93% (n=88/95) believing it would improve patient outcomes. - Local health systems should implement the national NMSC guideline once published.
96% (n=91/95) of surveyed skin cancer experts believe, if published, their local health system should adopt the national NMSC guideline. - NMSC should be established as a priority in national cancer policy, with tangible action taken in driving progress in NMSC.
65% (n=62/95) of skin cancer experts who responded to our survey felt NMSC is inadequately prioritised by NHS England. - Improvements in the quality and quantity of NMSC data should be prioritised.
66% (n=63/95) of skin cancer experts we surveyed stated poor data collection most impacted understanding of service demand. - The workforce crisis should be addressed to successfully improve NMSC patient care in the long-term.
88% (n=84/95) of respondent skin cancer experts agree there is a lack of capacity to manage the increasing demand for NMSC care, and increased referrals for NMSC services.
Driving action in NMSC among a multi-disciplinary group of experts
In January 2023, we hosted a roundtable discussion with a multi-disciplinary group of stakeholders to discuss the survey findings, and debate a way forward for making our recommendations a reality. The focus was on how to ensure a comprehensive, national clinical guideline and what streamlined implementation should look like to optimise outcomes. We are looking forward to further engagement in the future and advancing NMSC patient health for the better.
References
- National Cancer Registration and Analysis Service, Non-melanoma skin cancer in England, Scotland, Northern Ireland and Ireland. Available at: http://www.ncin.org.uk/publications/data_briefings/non_melanoma_skin_cancer_in_england_scotland_northern_ireland_and_ireland. Last accessed January 2023
- Melanoma UK, Non Melanoma Skin Cancer Report, March 2020. Available at: https://www.melanomauk.org.uk/non-melanoma-skin-cancer-report Last accessed: January 2023
- Cancer Research UK, Non-melanoma skin cancer statistics. Available at: https://www.cancerresearchuk.org/healthprofessional/cancer-statistics/statistics-by-cancer-type/nonmelanoma-skin-cancer#heading-One Last accessed: January 2023
- Goon et al, Predicted cases of U.K. skin squamous cell carcinoma and basal cell carcinoma in 2020 and 2025: horizon planning for National Health Service dermatology and dermatopathology, British Journal of Dermatology, 2017; 176:1351–1353. doi: 10.1111/bjd.15110
- Sanofi Data on File
- NHS. Overview: skin cancer (non-melanoma). Available at: https://www.nhs.uk/conditions/non-melanoma-skin-cancer/ Last accessed: January 2023
- Kent and Medway CCG, Dermatology Service Specifications. Available at: https://www.kentandmedwayccg.nhs.uk/application/files/6416/0025/0338/FOI.20.KAM036_-_Appendix_H.pdf Last accessed: January 2023
- London Cancer Alliance, Skin Stratified Pathway for Basal Cell Carcinomas. Available at: https://rmpartners.nhs.uk/wp-content/uploads/2017/03/appendix-12-skin-risk-stratified-pathway-forbcc-12_05_2015.pdf Last accessed: January 2023
- East and North Hertfordshire CCG, Skin Cancer (Including BCC) – Suspected. Available at: https://www.enhertsccg.nhs.uk/sites/default/files/pathways/Skin%20Cancer%20-%20Suspected.pdf Last accessed: January 2023
- NICE, Improving outcomes for people with skin tumours including melanoma (update), May 2010. https://www.nice.org.uk/guidance/csg8/resources/improving-outcomes-for-people-with-skintumours-including-melanoma-2010-partial-update-pdf-773380189 Last accessed: January 2023
- NICE, Suspected cancer: recognition and referral, June 2015. Available at: https://www.nice.org.uk/guidance/ng12/chapter/Recommendations-organised-by-site-of-cancer#skin-cancers Last accessed: January 2023
- Angus J, Diagnosis and management of nonmelanoma skin cancer. Prescriber. May 2017; 28(5):33-40. doi: https://doi.org/10.1002/psb.1572 Last accessed: January 2023
- 2022/23 priorities and operational planning guidance (2022) NHS choices. NHS. Available at: https://www.england.nhs.uk/publication/2022-23-priorities-and-operational-planning-guidance/. Last accessed: January 2023.
About the author
 Anju Bhalla, head of oncology & haemato-oncology, Sanofi UK & Ireland, has worked in the pharmaceutical industry for 25 years. She has held multiple sales and marketing roles, with vast specialty care experience.
Anju Bhalla, head of oncology & haemato-oncology, Sanofi UK & Ireland, has worked in the pharmaceutical industry for 25 years. She has held multiple sales and marketing roles, with vast specialty care experience.










