Experts warn of superbug risks after Madonna’s hospitalisation
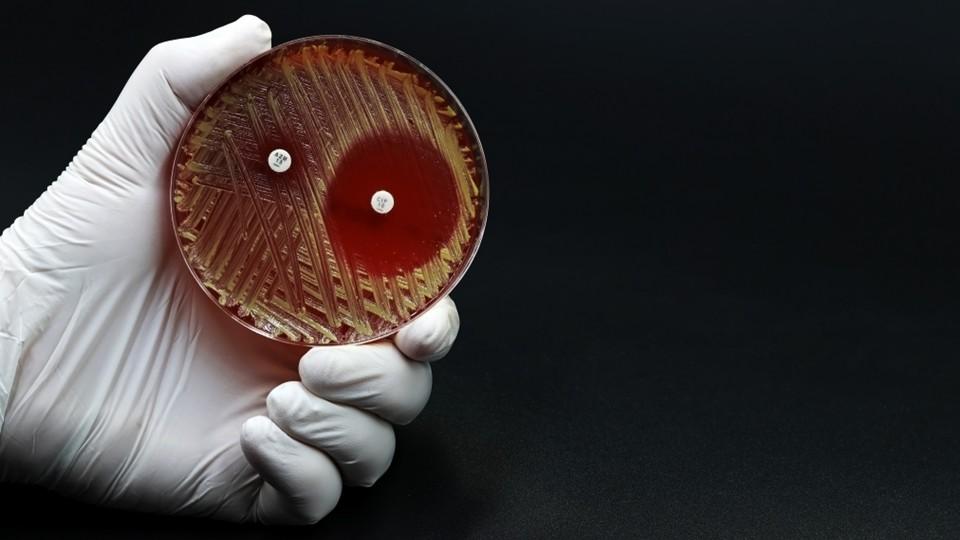
The recent hospitalisation of Madonna once again highlights the risks posed by bacterial infections and their potentially serious consequences for patients.
The 64-year-old pop superstar is understandably secretive about her health and details have been kept to a minimum while she recovers. Her manager, Guy Oseary, said in an Instagram post that the bacterial infection led to a stay of several days in intensive care, adding that her health is improving and a full recovery is expected. Since then, the Material Girl singer has issued a statement saying she is focusing on her recovery and is rescheduling her world tour to begin in October.
The real risk of antimicrobial resistance
It’s a high-profile example of the risks posed by bacterial infections, which can take hold in different parts of the body. Some large pharma companies ditched development of antibiotics over the last decade or so, although there are a few - such as Britain’s GSK - that continue to push forward with important R&D into a new generation of drugs. This situation is slowly improving, thanks to efforts by governments and health systems to incentivise research into new antibiotics targeting resistant strains – but there’s still a lot of work to be done.
The issue was highlighted by Lord O’Neill in an independent review on antimicrobial resistance commissioned by the UK government. The leading economist estimated that antimicrobial resistance (AMR) will cost the world an additional 10 million lives per year by 2050 - more than the number of people currently dying from cancer annually. AMR will also have a cumulative cost of $100 trillion, more than one and a half times the annual world GDP.
In 2019, the report led to the government producing a vision for AMR to be contained and controlled by 2040, with a five-year national action plan running until 2024.
Superbugs and sepsis
Three quarters of AMR or “superbug” infections are caused by just six bacterial strains, including Staphylococcus aureus (SA), the world’s most common cause of bacterial, post-surgical infection. Its “superbug” variant, MRSA, is the major cause of mortality. The other strains include Pseudomonas, Klebsiella, Streptococcus, E. coli, and Acinetobacter.
One potentially fatal result of infection is bacteraemia, where bacteria enter the bloodstream and overwhelm the body’s ability to fight off the infection. The infection is then able to spread throughout the body and can be fatal when the body responds with an extreme reaction known as sepsis. While sepsis can occur in anybody, including babies and children, the sick and elderly are more at risk, along with cancer patients and others whose immune systems are compromised.
Antibiotics are also used alongside most major surgical procedures to reduce the risk of infections setting in before and after operations.
Even fit and healthy people can be unlucky enough to pick up superbug infections, including athletes, with NFL players reporting MRSA skin infections. It demonstrates that no-one is entirely safe from this risk and superbugs threaten to set back medicine to the days before the discovery of penicillin, when injuries considered to be innocuous today could lead to life-threatening complications if bacteria entered a wound.
The case for a new generation of anti-infectives
Dr William Love is founder and chief scientific officer at Destiny Pharma, a company developing a new generation of anti-infectives - a catch-all term encompassing a range of medicines capable of stopping or killing the whole range of infectious organisms. Love pointed out that superbug infections can be picked up both inside and outside of hospital.
“Serious infections can start in almost any tissue in the body and the most common sites include the skin, the lungs, urinary tract and the gut,” Love said.
He continued: “Although serious and life-threatening in their own right, the stakes are raised once an established infection reaches the bloodstream. Bacterial sepsis is recognised as a number one priority to address by the World Health Organization.”
Destiny is one of a small group of companies developing new preventative treatments, but there is a pressing need for further interest in the sector to kick-start development of a new generation of drugs. Despite the issues with investment in research, these companies are pioneering a range of strategies to combat resistant microbes, including developing drugs that block resistance mechanisms to older antibiotics. Other strategies include drugs that disrupt or destroy the bacterial cell wall, the cell membrane within it, or stop bacteria producing chemicals that are essential for their survival.
Some companies are also trying to destroy bacteria by interfering with their DNA genetic code.
A question of price
With the G20 and influential figures attending the Davos Summit in 2018 recognising the threat posed by antibiotics, there is hope that new antibiotics will be approved and ready for use in hospital in the next few years.
The biggest problem holding back development is the low price commanded by antibiotics relative to drugs to treat other conditions such as cancer.
In the UK, the NHS is trying to introduce a subscription system where hospitals pay for new antibiotics against resistant bacteria, even if the drugs aren’t used. It’s a kind of insurance system, as new antibiotics are very much a last line of defence after older, cheaper drugs have not worked.
Destiny’s Love said more needs to be done: “While the new subscription system is a helpful step, action on many fronts needs to be supported, not least the development of novel anti-infectives, which can, in many circumstances, replace traditional antibiotics and counter the rising tide of antibiotic resistant infections.”