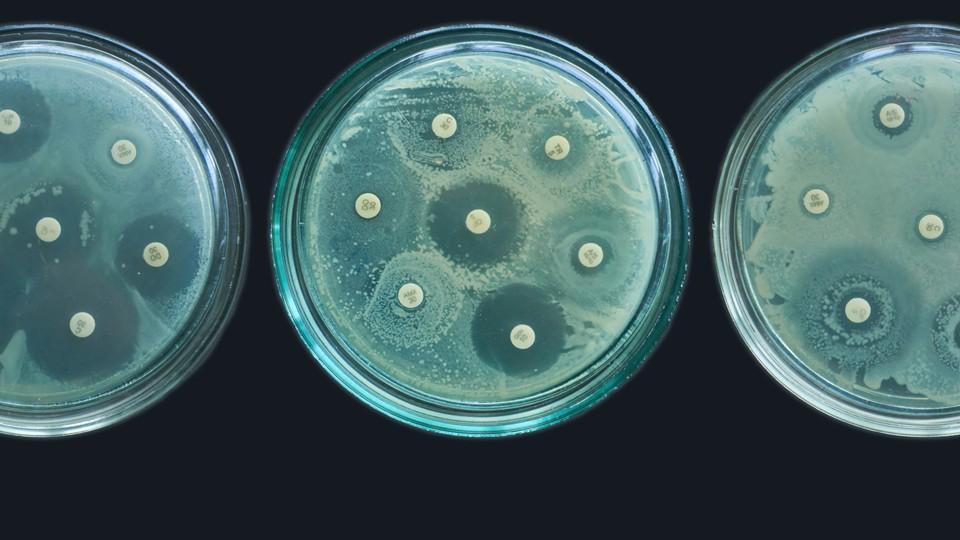
One world, one health: The interconnected web of antimicrobial resistance

Tackling antimicrobial resistance (AMR) requires a one health approach that joins the dots between the human, animal, and environmental drivers, consequences, and data.
AMR threatens to undermine “almost a century of health gains” and marshalling a response to such a problem “requires cooperation at many levels”.
That’s according to a newly published report from the US National Academies of Sciences, Engineering, and Medicine, which calls for a One Health approach that recognises the scale of the challenge, and the interconnectivity of its potential solutions.
“The COVID-19 pandemic has forced society to confront human vulnerability to microbial pathogens … in a way that has not been necessary in much of the world for a century,” said the authors, pointing to high levels of mortality linked to illnesses such as pneumonia, as well as surgery and childbirth, before the mass production of penicillin in the 1940s.
“The extent to which antimicrobial medicines changed these risks, though hard to overstate, is easily taken for granted.”
Growing threat of AMR
According to the Centers for Disease Control (CDC), antimicrobial-resistant pathogens cause 2.8 million human infections and 35,900 deaths every year in the US. And it costs $4.6 billion to treat just six of the most common resistant infections.
These stark figures are only set to get worse, with the World Health Organization predicting 50 million deaths a year by 2050, if the problem continues unheeded.
Yet efforts to mitigate the emergence and spread of resistant pathogens face a raft of challenges.
Progress is complicated by AMR being notoriously difficult to measure, and, although most obvious in human health, resistance emerges in animal health and in the environment.
“Better estimates of the burden of antimicrobial resistance in humans and animals depend on better microbiological data and more clarity on the appropriate design of epidemiological research.
“There are also challenges related to the complex adaptive nature of the problem. The same resistant infection can have drastically different consequences in humans and animals, depending on whether it is acquired in hospital or outside of it, in a high-income country or a low-income one.”
Success, then, will rely on an integrated response that focuses on surveillance, stewardship, and intervention accessibility across the spectrum of human, animal, and environmental health, said the report, which was commissioned to assess the progress of the 2014 National Strategy for Combating Antibiotic-Resistant Bacteria.
Surveillance
Among its raft of recommendations to governmental agencies, the report makes several aimed at strengthening and expanding surveillance processes.
“Surveillance systems are critically important for understanding the burden of antimicrobial resistance, detecting the emergence and spread of resistant pathogens, targeting interventions, and measuring their effectiveness,” it states.
Combining the AMR data collected by national and international organisations, including private industry, academic researchers, and disease-specific programmes, could offer “valuable insight into trends”.
It recommends the National Library of Medicine, which has already published “considerable information” on resistance genes, genome sequences, antimicrobial susceptibility data, and bacterial genomes, establish an open-source, unified AMR database.
“This database should support automatic importation from hospitals, laboratories and surveillance networks and link to genotypic data when available.”
Increasing the environmental isolates that are collected, and incorporating these into the proposed database, would contribute to a “more holistic understanding of AMR”.
“The Environmental Protection Agency should provide guidance and funding to states for testing point source discharge at wastewater treatment plants for AMR traits and integrating these data with other surveillance networks,” recommended the committee.
Stewardship
Effective stewardship is often cited as a key defence against AMR, and almost 90% of US hospitals now have CDC-inspired stewardship programmes in place – up from 40% in 2014.
Said the report: “Such rapid progress is heartening, but there are still many practice settings where the need for antimicrobial stewardship is pronounced.
“Nursing homes, dialysis centres, and long-term acute care hospitals all see considerable misuse and overuse of antimicrobials among patients who are, by definition, immunocompromised or infirm.”
As such, the report recommends that the Centers for Medicare and Medicaid Services require all such settings to implement stewardship programmes and publish the details on their Care Compare websites.
In addition, while many of the basic principles of antimicrobial stewardship are the same in human and animal medicine, the practice differs considerably in the two sectors, it said.
“The ability to track antimicrobial use is a key part of any stewardship programme, but the United States does not have a strong system to track antimicrobial use in animals.”
The FDA should, then, establish a process and clear metrics to facilitate better tracking of antimicrobial consumption in animals.
“This information would support the design and implementation of stewardship programmes.”
New agents: Development and accessibility
According to the report, the “mismatch between society’s need for new antimicrobials and industry’s willingness to invest in them” is an important barrier to tackling the growing threat of AMR.
“The medicines needed to treat resistant infections are complicated to develop and have a relatively small market both in terms of duration of use, usually only a few days, and need,” it said.
“When new antimicrobials are brought to market, good stewardship requires that older drugs be used first, even if there were no difference in price.”
The US’s current framework of ‘push’ and ‘pull’ incentives, designed to aid pharmaceutical companies to develop new antimicrobials, has contributed to a 10% increase in agents in the development pipeline, between 2014 and 2019.
“While this is a promising development, most of these products… do not appear to be meaningfully different from existing medicines,” said the report.
“Only six of the 50 anti-bacterials currently in the pipeline meet even one criterion for being innovative. Most of the antimicrobials approved recently offer little to no added clinical value over existing treatments.”
To incentivise the more targeted development of new agents, a Department of Health and Human Services (HHS) interagency committee should establish “objective criteria” to identify novel antimicrobials with the potential to fill critical, unmet needs.
“HHS should then support trials to establish the additional clinical benefit and optimal use of these drugs,” recommended the consensus report.
One health
In all, the report makes 14 recommendations, which together make up a global solution to a global problem.
Taking them from theory into practice will require large scale coordination across an increasingly large group of stakeholders, both in the US and overseas.
“By supporting a truly systemic, One Health response, the recommended programme may be able to drive progress on a range of health indicators, including, but not limited to, the burden of resistant infections,” concluded the authors.
About the author

Amanda Barrell is a freelance health and medical education journalist, editor and copywriter. She has worked on projects for pharma, charities and agencies, and has written extensively for patients, HCPs and the public.