Electrical implant treats severe depression in US patient
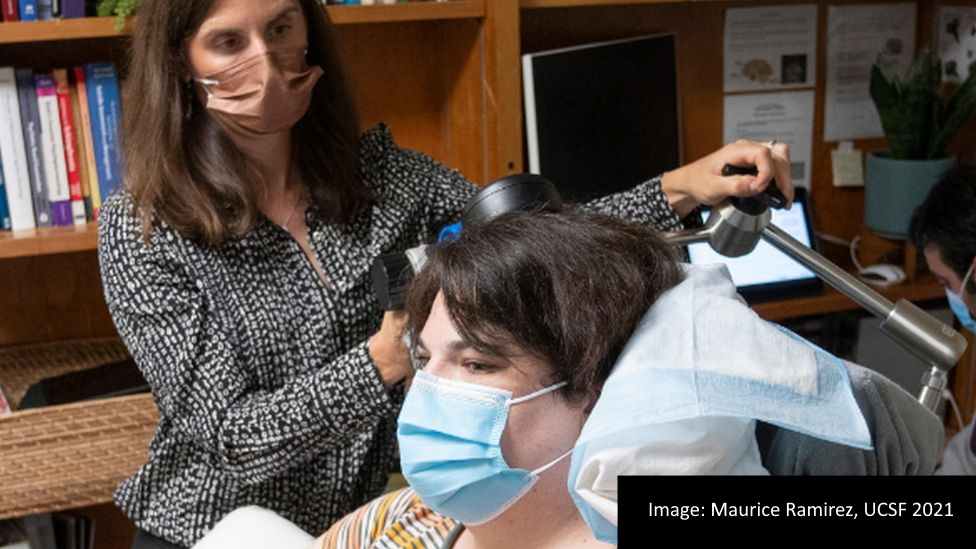
Researchers in the US have successfully treated a patient with severe depression via the use of an implant wired into the brain that interacts with a neural circuit linked to the disorder.
The team from University of California, San Francisco (UCSF) describe the implant as a "pacemaker" for the brain and – while it needs to be tested in additional patients – reckon it could represent a new way of treating psychiatric illness.
The matchbox-sized implant uses an approach called deep brain stimulation (DBS), which has previously been tested in clinical depression with disappointing results.
The UCSF scientists say one reason for the lacklustre effects to date is that implants have been targeted at a single area of the brain, delivering constant electrical stimulation.
In contrast, their device has been placed at the area of the brain that needs to be stimulated, and only acts when it detects a characteristic pattern – a neural biomarker – that indicates the onset of depressive symptoms.
The 36-year-old woman who received the implant has suffered severe depression since childhood that has resisted treatment with multiple antidepressant drugs and combinations, as well as electroconvulsive therapy (ECT).
"I was at the end of the line," said the patient, who has asked to be known only by her first name, Sarah.
"I was severely depressed," she added. "I could not see myself continuing if this was all I'd be able to do, if I could never move beyond this. It was not a life worth living."
Remarkably, the implant provided an almost immediate relief from symptoms, according to the researchers. One of the team – psychiatry professor Andrew Krystal – noted that antidepressants typically take several weeks to have an effect on mood.
"We've developed a precision-medicine approach that has successfully managed our patient's treatment-resistant depression by identifying and modulating the circuit in her brain that's uniquely associated with her symptoms," said Krystal.
https://www.youtube.com/watch?v=XCY8uQr2LKo
The researchers – who also include UCSF psychiatrist Katherine Scangos and neurosurgeon Edward Chang – used electrodes around Sarah's brain to identify the correct position for the implant, based signals seen when symptoms of depression were present.
Chang implanted then implanted NeuroPace's RNS System neurostimulation device, which is already FDA-approved to treat epilepsy. The case study has been published in the journal Nature Medicine.
Sarah has had the implant for a year, and reports that the improvement in symptoms was so abrupt she was fearful it could not maintained. "Now, those thoughts still come up, but it's just…poof…the cycle stops," she said.
"There's still a lot of work to do," acknowledges Scangos. "We need to look at how these circuits vary across patients and repeat this work multiple times. And we need to see whether an individual's biomarker or brain circuit changes over time as the treatment continues."
The team has already enrolled two other patients into the trial and intends to add nine more to establish proof-of-concept that could be taken forward into a double-blind, randomised controlled trial.














